What happens during a coronary angioplasty and how long does the procedure take?
The thought of ‘heart surgery’ usually conjures images of general anaesthetic, chest scars, and weeks of recovery. Coronary angioplasty (PCI) is entirely different. It is a minimally invasive procedure performed through a tiny pinhole in your wrist or groin, often allowing you to go home the same day.1 It relies on precision engineering rather than scalpel surgery, using fine wires to navigate the highways of your blood vessels while you chat with the doctor.
What We’ll Discuss in This Article
- The Setting: Why it happens in a ‘Cat Lab,’ not an operating theatre.
- Consciousness: Why you remain awake (and what you might feel).
- The Route: Wrist (Radial) vs. Groin (Femoral) access.
- The Mechanism: How a balloon and stent open a rock-hard blockage.
- Duration: Why it typically takes 30–60 minutes.
- The ‘Flutter’: Common sensations during the procedure.
- Immediate Recovery: Dealing with the puncture site.
Shutterstock
How long does it take?
A standard, uncomplicated angioplasty usually takes between 30 minutes and 2 hours.
- Diagnostic Angiogram Only: If they are just looking, it takes about 20–30 minutes.
- Stenting: If they proceed to treat a blockage, it adds another 30–60 minutes depending on the complexity of the plaque.
- Emergency: In a heart attack setting, the team works faster, often opening the artery within minutes of starting.
Step-by-Step: The Procedure
Preparation and Anaesthetic
You are taken to the ‘Catheterisation Lab’ (Cath Lab). It looks like an X-ray room. You will lie on a narrow table with an X-ray camera moving around you.
- Awake: You are not put to sleep. You remain awake to follow instructions (e.g., ‘take a deep breath’).
- Numbing: The cardiologist injects a local anaesthetic into your wrist (radial artery) or groin (femoral artery).2 This stings for 10 seconds, but then the area goes numb.
Access and Navigation
Once numb, a small tube (sheath) is inserted into the artery. This acts as the ‘doorway.’
- The Wire: A long, ultra-thin tube called a catheter is threaded through this sheath, up your arm, and into the opening of the coronary arteries.
- Sensation: You cannot feel the tube moving inside your body because blood vessels have no internal nerve endings. You might feel a dull pressure in your arm, but no sharp pain.
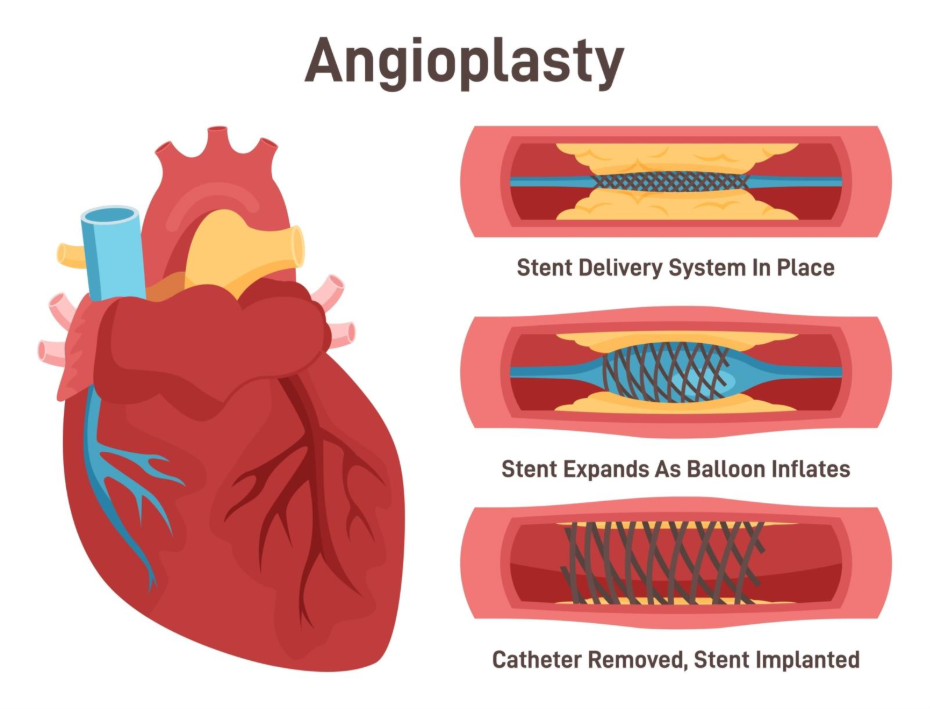
The Balloon and Stent
Once the catheter reaches the blockage, contrast dye is injected to make the artery show up on the screen.
- The Balloon: A fine wire is passed across the narrowing. A tiny balloon is slid over this wire and inflated at high pressure. This crushes the fatty plaque against the artery wall to make space.
- The Pain: When the balloon inflates, it temporarily stops blood flow completely. According to the British Heart Foundation, it is common to feel a brief ‘angina-like’ chest pain or discomfort at this exact moment, but it passes as soon as the balloon is deflated.
- The Stent: A metal mesh tube (stent) is usually crimped onto the balloon. When the balloon inflates, the stent expands and locks into place. The balloon is removed, but the stent stays there forever to keep the artery propped open.
What will I feel?
- The ‘Flutter’: You may feel palpitations or missed beats as the catheter touches the heart walls. This is normal.
- Warm Flush: When the dye is injected, many patients feel a sudden warm, ‘wet’ sensation spreading through their chest or groin. This is a harmless reaction to the contrast fluid.
- Pressure: You may feel the doctor pressing firmly on your wrist or groin at the start and end.
After the Procedure
Once the procedure is finished, the catheter is removed.
- Wrist (Radial): A tight compression band (like a thick wristwatch) is placed on your wrist to stop the bleeding. You can sit up immediately.
- Groin (Femoral): A plug or stitch is used, and you must lie completely flat for 2–4 hours to prevent bleeding.
Discharge
If the procedure was planned (elective) and successful, most patients go home the same day or the following morning. If you had a heart attack, you will stay in the hospital for a few days for monitoring.
Risks and Complications
While very safe, it is still an invasive procedure.
- Bruising: It is very common to have a large purple bruise at the wrist or groin.
- Bleeding: Rarely, the artery can bleed, requiring compression.
- Heart Attack: There is a tiny risk (less than 1%) that the procedure itself disturbs plaque and triggers a mild heart attack or requires emergency bypass surgery.
Conclusion
Coronary angioplasty is a marvel of modern medicine, fixing a life-threatening blockage via a tiny hole in the wrist in under an hour. The most painful part is usually just the initial ‘sting’ of the local anaesthetic. By staying calm and following the cardiologist’s instructions, you help the procedure go smoothly. Remember, the stent is now part of you, and maintaining it requires taking your antiplatelet medication exactly as prescribed.
Can I drive home?
No. You cannot drive immediately after the procedure. You must arrange for a lift. DVLA rules usually require you to stop driving for 1 week after a successful angioplasty.
Is the stent magnetic (MRI safe)?
Yes. Modern coronary stents are made of non-magnetic alloys (like cobalt-chromium). They are safe for MRI scans almost immediately, but always tell the radiographer.
Will the stent set off airport security?
No. The amount of metal is tiny, about the size of a small spring in a pen. It will not trigger metal detectors.
Can I eat before the procedure?
Usually, you are asked to fast (no food) for 4–6 hours beforehand, just in case of the rare event that you need urgent surgery or react to the medicine. You can usually drink water until 2 hours before.
What if I need the toilet during the procedure?
Try to go beforehand! However, if you are desperate during the procedure, tell the staff. They have bottles and pans and are used to this situation.
Does the stent move?
No. The stent is embedded into the artery wall under high pressure. Within weeks, your own skin cells grow over it, sealing it permanently into the tissue.
Can the artery block again?
Yes. This is called ‘Restenosis.’ It happens in about 5% of cases with modern drug-eluting stents. Taking your medication and quitting smoking are the best ways to prevent it.
Authority Snapshot
This article was written by Dr. Stefan Petrov, a UK-trained physician (MBBS) with extensive experience in acute hospital care. Having prepared countless patients for the catheter lab and managed their immediate recovery, Dr. Petrov demystifies the ‘plumbing’ of the heart. This content has been reviewed to ensure alignment with NHS and British Cardiovascular Intervention Society (BCIS) protocols, walking you through the procedure from the anaesthetic to the recovery room.

