What is the difference between a ‘normal irregular heartbeat’ and a dangerous arrhythmia?
It is a common human experience to occasionally feel a ‘skip,’ a ‘thump,’ or a brief fluttering sensation in the chest. While these ‘normal irregular heartbeats’ are often benign and related to lifestyle factors like caffeine or stress, they can sometimes signal an underlying clinical arrhythmia. Understanding the distinction is vital for maintaining cardiovascular health without unnecessary alarm. This article provides a clear, evidence-based breakdown of how the heart’s electrical system functions and how to recognise when an irregular rhythm requires professional medical evaluation.
What We’ll Discuss in This Article
- The clinical definition of heart palpitations versus clinical arrhythmias.
- Characteristics of a ‘normal’ irregular heartbeat, such as ectopic beats.
- Signs that indicate a heart rhythm may be medically dangerous.
- Common biological causes and external lifestyle triggers.
- The physiological differences between tachycardia and bradycardia.
- How to differentiate between anxiety-induced flutters and heart conditions.
- Essential safety guidance for emergency cardiac symptoms.
What is a Normal Irregular Heartbeat?
A ‘normal’ irregular heartbeat usually refers to isolated incidents where the heart’s rhythm is momentarily disrupted without affecting overall cardiac function. The most common form is an ectopic beat, where a premature signal causes the heart to feel like it has skipped a beat or added an extra one. According to NHS guidance, these are typically harmless and do not indicate underlying heart disease in most healthy individuals.
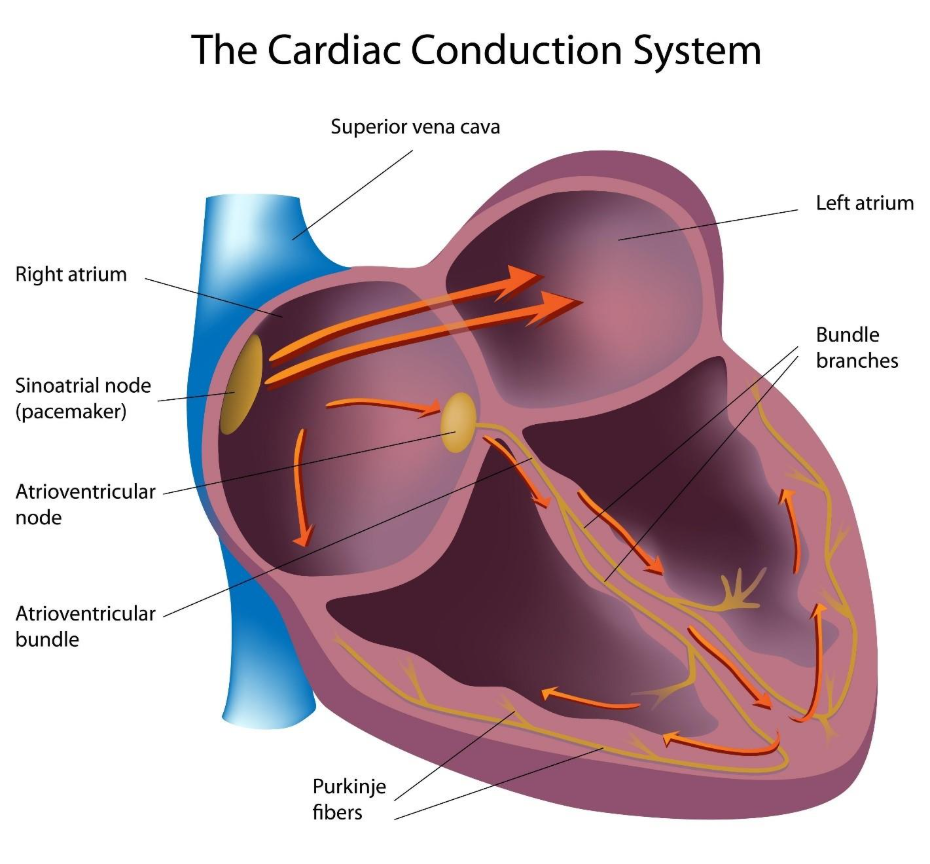
Expanded Explanation
Most ‘normal’ irregularities are actually palpitations—a term describing the awareness of your heartbeat. These sensations are usually brief and do not result in dizziness or fainting.
- Ectopic Beats: These occur when a part of the heart other than the natural pacemaker (the SA node) sends an electrical signal.
- Sinus Arrhythmia: A naturally occurring variation in heart rate that synchronises with your breathing; the heart speeds up slightly as you inhale and slows as you exhale.
- Transient Flutters: Brief sensations often triggered by a sudden surge of adrenaline or a heavy meal.
Clinical Context
In a healthy heart, these irregularities are self-correcting. The electrical system resets almost instantly, and the heart continues to pump blood effectively to the rest of the body. They are generally considered ‘normal’ if they occur infrequently and are not accompanied by systemic symptoms like chest pain or extreme fatigue.
What is a Dangerous Arrhythmia?
A dangerous arrhythmia is a persistent or severe disruption of the heart’s electrical signals that prevents the organ from pumping blood effectively. Unlike benign flutters, these conditions can lead to complications such as stroke, heart failure, or sudden cardiac arrest if the heart cannot maintain a coordinated rhythm. Clinical arrhythmias, such as Atrial Fibrillation or Ventricular Tachycardia, often require medical intervention to stabilise.
Indicators of Danger
A rhythm becomes ‘dangerous’ when it compromises the body’s oxygen supply. Key signs include:
- Persistence: The irregular rhythm lasts for several minutes or happens multiple times a day.
- Associated Symptoms: The irregularity occurs alongside breathlessness, lightheadedness, or ‘blacking out.’
- Structural Heart Issues: If you have a history of heart attacks or valve disease, any new irregularity is treated with higher clinical priority.
Safety Note
NICE guidance emphasises that conditions like Atrial Fibrillation (AF) significantly increase the risk of blood clots forming in the heart. If you feel a ‘persistently’ irregular pulse—one that feels like a ‘chaotic’ or ‘shuffling’ beat—it is important to have an ECG (electrocardiogram) to rule out AF.
Causes of Clinical Arrhythmias
Arrhythmias are often the result of structural changes to the heart muscle or the electrical pathways that coordinate the beat. These causes are typically internal and biological, requiring medical management.
- Coronary Artery Disease: Build-up of plaque in the arteries can starve the heart of oxygen, damaging the electrical nodes.
- Cardiomyopathy: Diseases of the heart muscle that cause it to become enlarged, thick, or rigid, disrupting electrical conduction.
- Electrolyte Imbalances: Abnormal levels of potassium, sodium, or magnesium in the blood can interfere with the electrical ‘firing’ of heart cells.
- Heart Valve Disorders: When valves don’t close properly, the heart must work harder, leading to chamber enlargement and rhythm disturbances.
- Congenital Defects: Some individuals are born with extra electrical pathways (such as in Wolff-Parkinson-White syndrome).
Triggers for Heart Palpitations
In contrast to the structural causes of arrhythmias, heart palpitations are often provoked by external triggers. These are factors that stimulate the nervous system or temporarily stress the heart.
- Stimulants: High intake of caffeine (coffee, energy drinks), nicotine, and certain over-the-counter cold remedies containing pseudoephedrine.
- Emotional Stress: Anxiety and panic attacks trigger the ‘fight or flight’ response, releasing adrenaline that increases heart rate and sensitivity to ectopic beats.
- Alcohol and Drugs: Alcohol can irritate the heart’s electrical system; some people experience ‘Holiday Heart Syndrome’ after heavy drinking episodes.
- Dehydration and Fatigue: A lack of fluids or extreme exhaustion can make the heart more prone to minor rhythm fluctuations.
- Hormonal Changes: Periods of significant hormonal shift, such as pregnancy or menopause, are frequent triggers for increased palpitations.
Differentiation: Palpitations vs. Arrhythmia
Differentiating between a harmless palpitation and a clinical arrhythmia involves looking at the duration, frequency, and systemic impact of the sensation.
| Feature | Normal Palpitation / Ectopic | Dangerous Arrhythmia |
| Duration | Lasts seconds to a few minutes. | Can last for hours or be permanent. |
| Rhythm | Usually a single ‘thump’ or brief race. | Often feels chaotic, persistent, or very slow. |
| Physical Impact | No dizziness or fainting. | Often causes lightheadedness or syncope. |
| Trigger | Often linked to caffeine or stress. | Often occurs at rest for no clear reason. |
| Recovery | Feels normal immediately after. | May leave the person feeling weak or breathless. |
The ‘Pulse Test’
A helpful way to differentiate is by checking your pulse at the wrist. A normal irregularity feels like a steady rhythm with an occasional ‘early’ beat. A dangerous arrhythmia, particularly Atrial Fibrillation, will feel completely irregular, with no detectable pattern or steady beat at all.
Conclusion
Distinguishing between a normal irregular heartbeat and a dangerous arrhythmia is key to proactive heart health. While most flutters are benign responses to lifestyle triggers like stress or stimulants, any irregularity accompanied by dizziness, chest pain, or a persistent ‘chaotic’ rhythm requires investigation. Understanding your own ‘normal’ and monitoring for systemic symptoms can provide peace of mind and ensure timely medical support when needed.
If you experience severe, sudden, or worsening symptoms, call 999 immediately.
Can anxiety cause a dangerous arrhythmia?
Anxiety causes palpitations, which are usually harmless, but chronic stress can contribute to long-term heart strain; however, it rarely causes a dangerous arrhythmia in a healthy heart.
How many ectopic beats a day is normal?
Most people have several hundred ectopic beats a day without knowing it; they only become a concern if they make up a high percentage of your total daily heartbeats.
Is Atrial Fibrillation (AF) always a medical emergency?
AF is a serious condition that requires medical management to prevent stroke, but it is often a chronic condition rather than an immediate 999 emergency unless accompanied by chest pain.
Does caffeine cause permanent heart damage?
No, caffeine is a temporary stimulant that triggers flutters; once it leaves your system, the heart rhythm typically returns to its baseline.
Can I have a dangerous arrhythmia without feeling any symptoms?
Yes, some arrhythmias are ‘silent’ and are only discovered during routine medical exams or after a complication occurs.
What is the best way to record an irregular rhythm for a doctor?
Using a wearable heart monitor or keeping a ‘symptom diary’ detailing what you were doing when the irregularity started can be very helpful for clinical review.
Authority Snapshot (E-E-A-T Block)
This article was written by Dr. Rebecca Fernandez, a UK-trained physician with an MBBS and extensive clinical experience across cardiology, emergency medicine, and internal medicine. In this guide, we will explore the nuances between benign heart flutters and clinical arrhythmias to help you understand when medical attention is necessary. This information adheres to NHS and NICE standards to ensure the highest levels of accuracy and safety.

