Can anxiety or panic attacks be confused with arrhythmias?
The relationship between the mind and the heart is one of the most powerful and complex systems in the human body. When you experience intense anxiety or a panic attack, your brain signals a massive release of adrenaline, which immediately causes your heart to race, pound, or flutter. Because these sensations are identical to the symptoms of a heart rhythm disorder, many people find themselves in a state of double distress, wondering if they are experiencing a psychological event or a life-threatening cardiac emergency. Differentiating between the two is a common clinical challenge, even for experienced healthcare professionals. Understanding the nuances of how anxiety affects your pulse is the first step in finding the right management path. This article explores the physiological overlap between panic and palpitations, providing a medically neutral guide to help you understand what is happening in your body.
What We’ll Discuss in This Article
- The clinical overlap between anxiety symptoms and heart rhythm disturbances.
- Why the body’s ‘fight or flight’ response mimics a cardiac arrhythmia.
- Identifying the specific physical sensations of a panic-led racing heart.
- How chronic anxiety can act as a direct trigger for real electrical heart issues.
- The biological mechanisms that link the brain’s stress centres to the heart’s pacemaker.
- Practical ways to differentiate between a panic attack and a clinical arrhythmia.
- Emergency safety guidance for sudden or severe chest and heart symptoms.
Can Anxiety or Panic Attacks be Confused With Arrhythmias?
Yes, anxiety and panic attacks are frequently confused with arrhythmias because they share almost identical physical symptoms. During a panic attack, the heart rate often climbs to over 100 beats per minute, which is clinically defined as tachycardia. According to NHS guidance, the physical manifestations of panic, including chest tightness, breathlessness, and a pounding heart, are so intense that they are often mistaken for a heart attack or a serious heart rhythm problem.
Expanded Explanation
The confusion arises because both conditions involve the same final pathway: the heart’s electrical system.
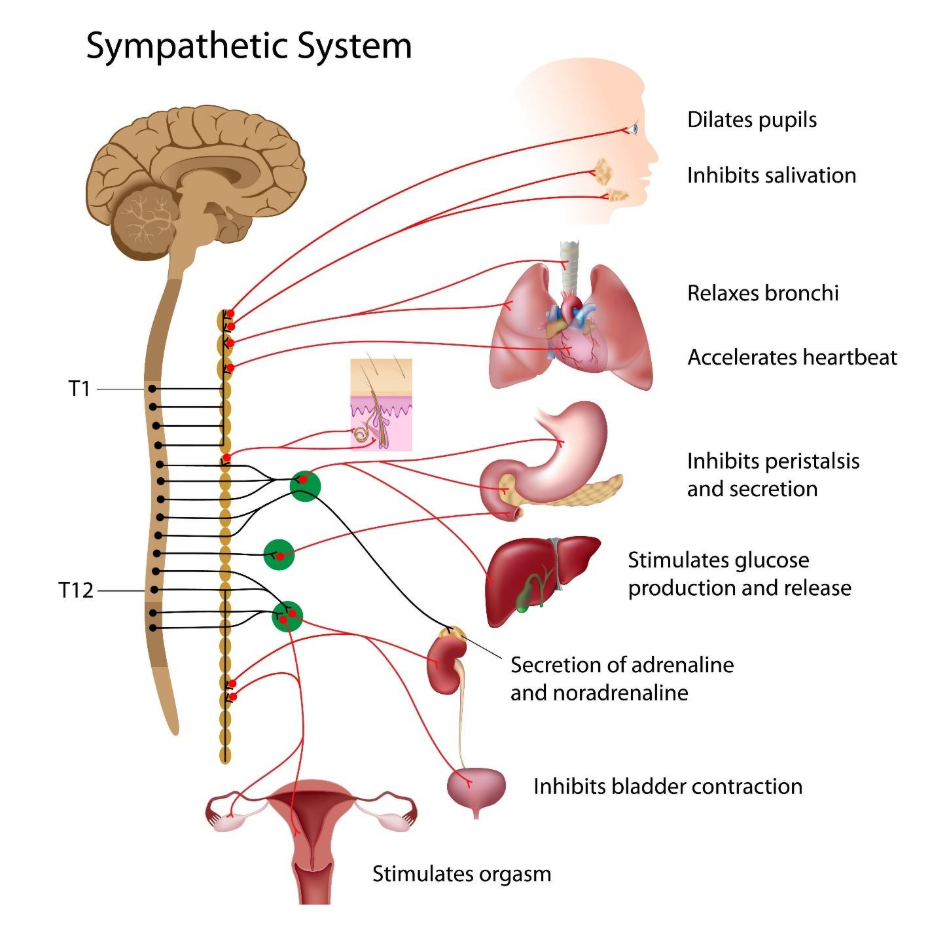
- The Adrenaline Surge: In anxiety, the brain’s amygdala triggers the sympathetic nervous system. This floods the heart with adrenaline, forcing it to beat faster and harder.
- Hyperventilation: Anxiety often causes fast, shallow breathing. This changes the carbon dioxide levels in your blood, which can cause chest pain and tingling sensations, further mimicking heart trouble.
- The Feedback Loop: If you feel a palpitation due to stress, the fear of that sensation causes more adrenaline to be released, which in turn makes the heart beat even faster, creating a self-sustaining cycle.
Clinical Context
In UK emergency departments, many patients presenting with suspected heart rhythm issues are found to be experiencing a panic attack. However, because anxiety can also be a symptom of a real arrhythmia, such as the sudden onset of Atrial Fibrillation, clinicians must be careful to rule out a cardiac cause before concluding that the issue is purely psychological.
How Does Anxiety Affect the Heart’s Rhythm?
Anxiety affects the heart by increasing the ‘automaticity’ of its electrical cells. This means that the heart muscle becomes more sensitive to every signal, making it more likely to fire off extra or premature beats. While the heart remains structurally healthy during a panic attack, the electrical timing is temporarily shifted into a state of ‘high alert’, resulting in a very fast but usually regular rhythm.
Impact on Cardiac Function
- Sinus Tachycardia: This is the most common finding during anxiety. The heart rate is fast, but it is still being controlled by the heart’s natural pacemaker, the SA node.
- Increased Force of Contraction: Adrenaline makes the heart muscle squeeze more powerfully, which is why you feel the ‘pounding’ against your ribs or in your throat.
- Temporary Blood Pressure Rise: The stress response causes blood vessels to constrict, which raises blood pressure and can make the heartbeat feel even more forceful and noticeable.
Safety Note
NICE guidance suggests that if you have a known heart condition, the stress of an anxiety attack could potentially trigger a more serious arrhythmia, such as Atrial Fibrillation. Therefore, it is important to manage both the heart rhythm and the underlying anxiety to prevent this cross-over.
Causes of Overlapping Symptoms
The reason the two conditions are so hard to distinguish is that they involve the same biological mechanisms.
- The Vagus Nerve: This nerve connects the brain and the heart. High stress can irritate the vagus nerve, causing the heart to skip beats or suddenly race.
- Chest Wall Tension: Anxiety causes the muscles around the ribs to tighten, creating a ‘heavy’ chest feeling that is easily confused with cardiac pressure.
- Adrenal Gland Activity: Panic attacks cause a sudden ‘dump’ of catecholamines (like adrenaline), which directly stimulates the heart’s electrical pathways.
- Blood Chemistry Changes: Rapid breathing during panic (hyperventilation) alters calcium and potassium levels momentarily, which can cause benign but frightening heart flutters.
Triggers for Anxiety and Arrhythmias
Many external factors can simultaneously trigger both a panic response and a heart rhythm irregularity, making it difficult to isolate the cause.
- Caffeine and Nicotine: These are dual-purpose triggers; they stimulate the brain’s anxiety centres and the heart’s electrical nodes at the same time.
- Sleep Deprivation: A lack of sleep makes the brain more prone to panic and the heart more prone to electrical skips (ectopic beats).
- Dehydration: This causes the heart to race to maintain blood pressure, which can then trigger a panic attack in someone who is sensitive to their heartbeat.
- Specific Medications: Some asthma inhalers or decongestants can cause a racing heart as a side effect, which can be interpreted by the brain as a sign of panic.
Differentiation: Panic Attack vs. Arrhythmia
While the sensations are similar, there are key differences in how these two events typically behave.
| Feature | Panic Attack | Clinical Arrhythmia |
| Onset | Usually builds up over a few minutes. | Often starts instantly in a single beat. |
| Rhythm | Fast but usually very regular. | Often feels chaotic, ‘shuffling’, or irregular. |
| Resolution | Slows down gradually as you calm. | May stop instantly or ‘snap’ back to normal. |
| Physical Signs | Tingling hands, sweating, shaking. | Fainting, near-fainting, or grey skin. |
| Trigger | Often linked to a thought or stressor. | Often occurs with no emotional trigger. |
The ‘Pulse Check’
Checking your pulse during an episode is the most effective way to help your doctor. If the pulse is fast but as steady as a drumbeat, it is more likely to be a sinus tachycardia related to anxiety. If the pulse is fast and feels completely random or chaotic (like a ‘bag of worms’), it is more likely to be a clinical arrhythmia like Atrial Fibrillation.
Conclusion
Anxiety and panic attacks are frequently confused with arrhythmias because they both utilise the same electrical and hormonal pathways in the body. While a panic attack can make you feel as though your heart is failing, it is usually a healthy response to a perceived threat, resulting in a fast but regular heart rate. Conversely, a true arrhythmia is a technical malfunction in the heart’s wiring. Distinguishing between the two requires a calm assessment of the rhythm’s ‘tempo’ and the presence of any accompanying symptoms like fainting. Most importantly, since the two conditions can coexist and exacerbate one another, seeking a clinical review ensures that both your heart health and your mental well-being are properly supported.
If you experience severe, sudden, or worsening symptoms, call 999 immediately.
Can a panic attack actually cause a heart attack?
In a person with a healthy heart, a panic attack is very unlikely to cause a heart attack, though the physical sensations are remarkably similar.
Why do I feel palpitations when I’m not even feeling stressed?
You may be experiencing ‘subconscious’ stress, or you may be having a clinical arrhythmia that has nothing to do with your emotions.
Can an arrhythmia make me feel like I’m having a panic attack?
Yes, a sudden fast heart rate can trigger the body’s ‘fight or flight’ response, making you feel anxious or panicked as a result of the heart rhythm.
Is it dangerous if my heart rate stays high after a panic attack?
It is normal for the heart rate to take some time to settle after a surge of adrenaline, but if it remains over 100 bpm for hours, you should consult a doctor.
How does deep breathing help a racing heart?
Slow, deep breathing stimulates the parasympathetic nervous system (the ‘rest and digest’ system), which sends a signal to the heart to slow down.
Can dehydration cause both anxiety and heart flutters?
Yes, dehydration puts the body under physical stress, which can lead to both increased anxiety and an irritable heart rhythm.
Authority Snapshot (E-E-A-T Block)
This article was written by Dr. Rebecca Fernandez, a UK-trained physician with an MBBS and extensive experience in both cardiology and psychiatry. Having managed acute cardiac cases and provided evidence-based psychological therapies, Dr. Fernandez is uniquely positioned to explain the intersection of mental well-being and heart health. This guide follows NHS and NICE standards to provide a safe, accurate, and reassuring overview of how to distinguish between emotional distress and heart rhythm disorders.

