When is Mitral Valve Repair Better Than Replacement?
When a mitral valve becomes significantly leaky (regurgitation) or narrowed (stenosis), intervention is often necessary to prevent heart failure. In the UK, the two primary surgical options are repairing the existing valve or replacing it with an artificial one. While both procedures aim to restore proper blood flow, clinical guidelines generally favour repair whenever possible. Repairing the valve allows a patient to keep their own living tissue, which often leads to better heart function and a lower risk of long-term complications. This article explores when and why a repair is superior to a replacement and what factors influence the surgeon’s decision.
What We’ll Discuss in This Article
- The clinical advantages of repairing a natural valve over replacing it.
- Why repair is the ‘gold standard’ for degenerative mitral regurgitation.
- The impact of valve repair on long-term heart muscle function.
- Situations where replacement becomes the more appropriate choice.
- The differences in recovery and lifelong medication requirements.
- How the ‘heart team’ decides the best approach for each patient.
When Mitral Valve Repair Is the Preferred Option?
Mitral valve repair is considered better than replacement for most patients with ‘primary’ mitral regurgitation, particularly when caused by mitral valve prolapse. Repair is superior because it preserves the heart’s natural anatomy, maintains the strength of the left ventricle, and eliminates the need for lifelong blood-thinning medication (warfarin). Clinical data consistently shows that patients who undergo successful repair have better long-term survival rates and a lower risk of heart infection (endocarditis) compared to those who receive a replacement.
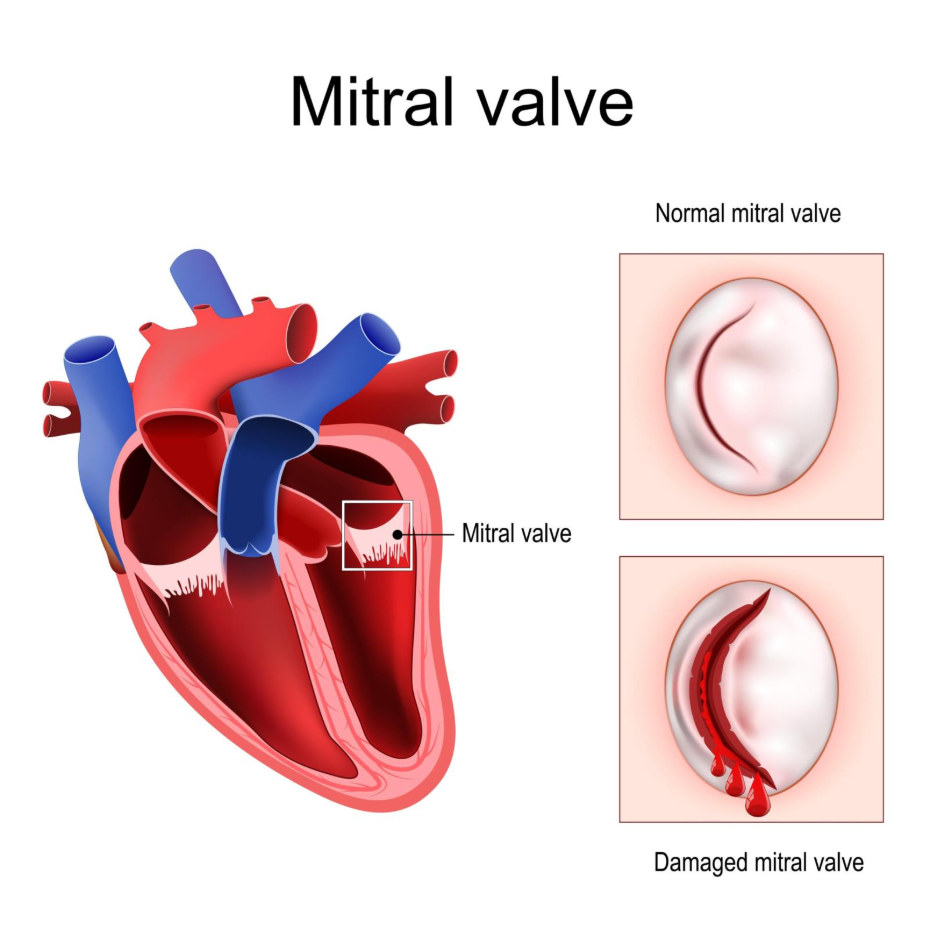
In the UK, NICE guidelines recommend that if a valve can be reliably repaired, it should be the first choice. Surgeons aim for a repair whenever the valve leaflets are flexible and the underlying structure of the heart is strong enough to support the reconstructed valve.
- Preserves Anatomy: Keeping the ‘chordae tendineae’ (heart strings) intact supports heart shape.
- No Warfarin: Unlike mechanical replacements, repairs do not require permanent anticoagulation.
- Durability: A successful repair often lasts a lifetime, whereas biological replacements may wear out.
- Better Outcomes: Higher long-term survival and lower risk of stroke and infection.
Why is Preserving the Heart Muscle Important?
The primary reason repair is superior is the preservation of the ‘subvalvular apparatus’ the network of strings (chordae) and muscles (papillary muscles) that connect the valve to the heart wall. When a valve is replaced, these connections are often cut. Because these strings act like internal ‘tethers’ that help the heart maintain its elliptical shape, losing them can cause the heart to become more spherical and lose its pumping efficiency over time.
By repairing the valve, the surgeon keeps these tethers in place. This ensures the left ventricle stays strong and reduces the likelihood of developing heart failure years after the surgery.
What are the Main Causes for Choosing Repair?
The main cause for choosing repair is ‘degenerative’ valve disease, such as Mitral Valve Prolapse or Barlow’s Syndrome. In these cases, the valve tissue is usually healthy enough to be reshaped. Surgeons can trim away excess tissue, reinforce the valve ring (annuloplasty), or even create new ‘artificial’ heart strings to ensure the valve closes tightly again.
- Annuloplasty: Placing a metal or fabric ring around the valve to tighten the opening.
- Leaflet Resection: Removing a small piece of a floppy leaflet so the edges meet perfectly.
- Artificial Chords: Using Gore-Tex threads to replace broken or stretched natural strings.
What are the Triggers for Choosing Replacement Instead?
While repair is preferred, certain triggers make replacement the safer or only option. If the mitral valve is heavily calcified (hardened like bone) or has been severely damaged by an infection like endocarditis, it may be impossible to reshape it reliably. In these instances, a replacement is necessary to ensure the patient does not leave the operating theatre with a still-leaking valve.
- Severe Calcification: Often seen in rheumatic heart disease or elderly patients.
- Infective Endocarditis: If the bacteria have ‘eaten’ holes in the valve leaflets.
- Failed Previous Repair: If a previous attempt to fix the valve has not lasted.
- Technical Complexity: If the damage is spread across too much of the valve for a stable repair.
Differentiation: Repair vs. Mechanical vs. Biological Replacement
It is important to differentiate between the three main outcomes of mitral surgery. A repair is the use of your own tissue. If replacement is needed, you must choose between a ‘mechanical’ valve (made of carbon and metal) or a ‘biological’ valve (made from pig or cow tissue). Each has distinct trade-offs regarding durability and the need for medication.
| Feature | Mitral Valve Repair | Mechanical Replacement | Biological Replacement |
| Tissue Used | Your own. | Metal/Carbon. | Animal tissue. |
| Blood Thinners | Short-term or none. | Lifelong (Warfarin). | Short-term only. |
| Durability | Very high/Lifelong. | Permanent. | 10–15 years. |
| Heart Strength | Best preserved. | Slightly reduced. | Slightly reduced. |
Conclusion
Mitral valve repair is the gold standard of treatment for most patients with a leaky mitral valve. By preserving the heart’s natural structure and avoiding the complications of artificial valves and long-term blood thinners, repair offers the best long-term prognosis and quality of life. While replacement remains a vital and life-saving backup for valves that are too damaged to fix, the goal of modern UK cardiac surgery is to ‘repair rather than replace’ whenever possible.
If you experience severe, sudden, or worsening symptoms, such as intense chest pain, sudden breathlessness, or fainting, call 999 immediately.
Is mitral valve repair a bigger operation than replacement?
Technically, a repair can be more complex and take slightly longer for the surgeon to perform, but for the patient, the recovery process and hospital stay are very similar.
Can all surgeons perform mitral valve repair?
While most cardiac surgeons can perform replacements, complex repairs are often referred to specialist ‘mitral centres’ with higher volumes of these specific procedures.
How long does a repaired mitral valve last?
Can I have a repair if my valve is narrowed (stenosis)?
Repair is much more common for a leaky valve (regurgitation); narrowed valves usually require replacement or a ‘balloon’ procedure to stretch them open.
Will I be able to exercise after a repair?
Yes, once you have recovered from surgery (usually 6–12 weeks), most patients can return to full physical activity and often feel more energetic than before.
What is a ‘MitraClip’?
The MitraClip is a less-invasive way to repair the valve using a catheter through the groin, usually reserved for patients too frail for open surgery.
Authority Snapshot (E-E-A-T Block)
This article has been reviewed by Dr. Stefan Petrov, a UK-trained physician with an MBBS and postgraduate certifications in Basic Life Support (BLS) and Advanced Cardiac Life Support (ACLS). Dr. Petrov has extensive clinical experience in general medicine and surgical settings, including the management of patients undergoing cardiac valve interventions. This guide follows NHS and NICE principles to explain the clinical decision-making process between mitral valve repair and replacement.

