Why does joint pain worsen with activity?
The experience of joint pain intensifying during or after physical activity is one of the most common challenges for those living with osteoarthritis. This occurs because the protective mechanisms that usually ensure smooth, painless movement have been compromised by the thinning of the articular cartilage. In a healthy joint, this cartilage acts as a highly efficient shock absorber and a friction-reducing surface, but as it becomes uneven or thinner, the mechanical forces of movement are distributed less effectively. Every step, lift, or twist can lead to increased pressure on the sensitive bone underneath and the surrounding joint lining, triggering the characteristic dull ache or sharp twinges associated with the condition. While it may feel logical to avoid movement to prevent this discomfort, understanding the biological and mechanical reasons why activity increases pain is the first step toward finding a balance that supports joint health. By learning how to manage the load on your joints and strengthening the supporting muscles, you can continue to stay active while minimising the impact on your comfort.
What We’ll Discuss in This Article
- The loss of cartilage as a shock absorber and its impact on movement
- How mechanical friction and bone-on-bone contact trigger pain signals
- The role of joint pressure and the sensitivity of the subchondral bone
- How activity-induced inflammation affects the joint lining (synovium)
- Why muscle fatigue leads to increased joint stress during exercise
- Identifying specific triggers and activities that increase joint load
- The importance of balancing activity with rest to support joint repair
The loss of shock absorption
In a healthy joint, the ends of the bones are covered in a layer of articular cartilage that is incredibly smooth and resilient. This tissue is designed to absorb the impact of our movements, acting like a spring that compresses and rebounds with every step. In osteoarthritis, this cartilage becomes thinner, less elastic, and may develop small cracks or pits.
When you engage in physical activity, the force of your body weight must still be absorbed. Because the cartilage is no longer performing its job effectively, more of that force is transmitted directly to the bones. This increased mechanical stress is detected by the dense network of nerves in the joint, resulting in a dull, deep ache. The NHS explains that this is why pain is often felt most acutely during weight-bearing activities like walking or running, where the joints are under the most pressure.
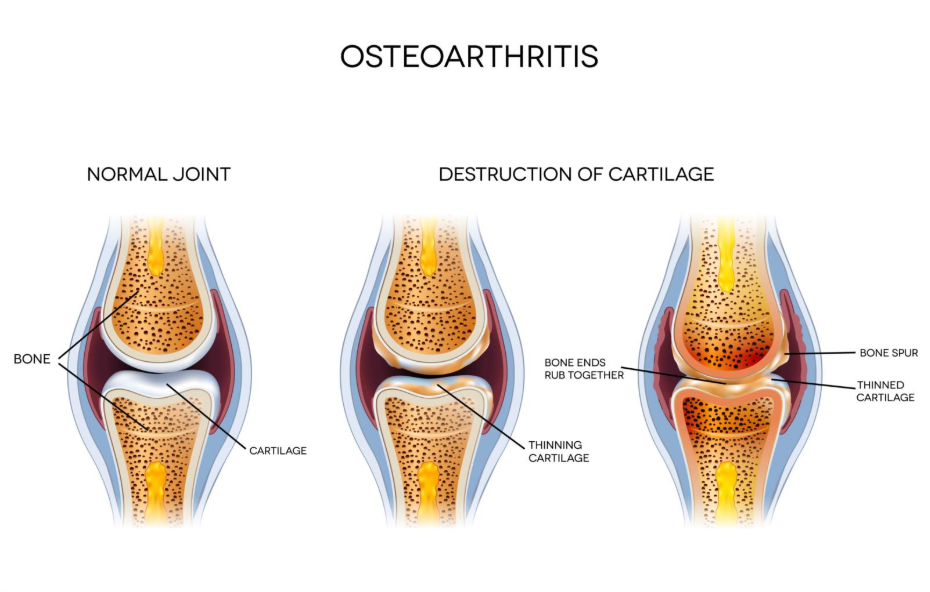
Mechanical friction and the subchondral bone
As the cartilage protective layer diminishes, the surfaces of the bones can begin to come into closer contact with one another. Unlike cartilage, bone is highly sensitive and contains many pain fibres. When the joint moves, the rougher surfaces of the thinning cartilage or the exposed bone create mechanical friction.
This friction does more than just cause immediate discomfort; it also irritates the subchondral bone (the bone directly beneath the cartilage). In response to this increased pressure, the bone often becomes thicker and harder, a process known as subchondral sclerosis. During activity, the rubbing and pressure on these sensitive bone surfaces send sharp pain signals to the brain. This is often the cause of the ‘twinges’ or ‘stabbing’ sensations that people feel when they move a joint through its full range of motion.
Activity-induced inflammation of the joint lining
Physical activity can also trigger low-grade inflammation within the joint, a condition known as synovitis. When an osteoarthritic joint is used, tiny microscopic fragments of cartilage or bone can break off into the joint space. The synovium (the lining of the joint) attempts to clear these fragments away, but this process can cause the lining to become inflamed and swollen.
This inflammatory response is why pain often persists or even increases after you have finished an activity. The inflammation makes the entire joint more sensitive, meaning that even light movements can feel painful for several hours or days following overexertion. Clinical guidance from NICE suggests that managing this localized irritation, often through cold therapy or short periods of rest, is essential for recovering from activity-induced flare-ups.
The role of muscle fatigue and joint stability
The muscles surrounding a joint act as its primary external stabilisers and additional shock absorbers. When you are active, these muscles work to take the strain off the joint itself. However, as an activity continues and the muscles begin to fatigue, they become less effective at providing this support.
Once the muscles tire, the joint must absorb a much higher percentage of the mechanical load. This lead to a significant increase in pain toward the end of a long walk or a busy day of housework. Many people with osteoarthritis have some degree of muscle weakness because they have subconsciously avoided using the painful joint. This creates a cycle where weak muscles lead to more joint pain during activity, which then leads to further muscle weakness. Strengthening these supporting muscles is one of the most effective ways to reduce activity-related pain.
Investigating the triggers for increased joint load
Not all activities are equal when it comes to joint pain. Certain movements put significantly more stress on an osteoarthritic joint than others. Identifying these high-load triggers can help you modify your movements to stay active without excessive discomfort.
Common high-load triggers include:
- High-impact movements: Jumping, running, or skipping, which send a sudden force through the joint.
- Stair climbing: Going down stairs, in particular, puts a force several times your body weight through the knee joint.
- Repetitive twisting: Movements like pivoting on one leg or twisting at the waist during gardening.
- Prolonged standing: This puts a constant, static load on the hips and knees, which can be more painful than gentle walking.
Identifying triggers for symptom flare-ups
A flare-up is often the body’s reaction to a sudden spike in joint load. For example, a person who usually walks for 20 minutes might experience a significant increase in pain if they suddenly attempt a 60-minute hike. The joint tissues, which are already struggling with the ‘wear and repair’ cycle, become overwhelmed by the sudden increase in demand. Other triggers include wearing unsupportive footwear, which fails to help the joint with shock absorption, or carrying heavy loads like grocery bags, which adds immediate mechanical pressure to the affected areas.
Differentiation: Activity pain in OA vs Inflammatory Arthritis
It is important to distinguish the pain of osteoarthritis from that of inflammatory conditions like rheumatoid arthritis. In osteoarthritis, pain almost always gets worse with more activity and improves with rest. In contrast, the pain and stiffness of rheumatoid arthritis often feel better with movement and are at their most severe after periods of rest, such as first thing in the morning. If your joint pain significantly improves with activity rather than worsening, it may be a sign of an inflammatory or autoimmune condition, which requires a different medical management approach.
Conclusion
Joint pain worsens with activity in osteoarthritis because the loss of protective cartilage leaves the sensitive bone surfaces and joint lining exposed to increased mechanical stress and friction. When the body’s natural shock absorbers are compromised, every movement requires the joint and its surrounding muscles to work harder. While this pain can be discouraging, it is a signal to manage the ‘load’ on the joint rather than to stop moving entirely. By focusing on low-impact activities, building muscle strength to support the joint, and avoiding sudden spikes in intensity, individuals can stay mobile while keeping their discomfort at a manageable level. Balancing active movement with appropriate rest allows the joint’s repair mechanisms to function more effectively, supporting long-term joint health.
If you experience severe, sudden, or worsening symptoms, call 999 immediately.
Why does my pain stay for hours after I stop moving?
This is usually due to localized inflammation (synovitis) of the joint lining, which stays irritated as it tries to clear away fragments of cartilage and bone debris.
Is it safe to ‘push through’ the pain?
Generally, it is better to listen to your body. While mild aching is common, sharp or increasing pain is a sign to rest or switch to a lower-impact movement.
Why is walking down stairs more painful than walking up?
Walking down stairs requires your muscles to control your descent, which puts significantly more pressure on the knee joint and its cartilage.
Does carrying extra weight make the activity pain worse?
Yes, every extra pound of body weight significantly multiplies the pressure on your weight-bearing joints during movement.
Will my joints eventually stop hurting when I exercise?
As your supporting muscles get stronger, they will take more of the load, which often leads to a significant reduction in pain during daily activities.
Should I always rest if a joint is painful?
No, prolonged rest can lead to joint stiffness and muscle weakness. The goal is to find a balance of gentle, low-impact movement.
Authority Snapshot
This article was written by Dr. Stefan Petrov, a UK-trained physician with an MBBS and postgraduate certifications including Basic Life Support (BLS), Advanced Cardiac Life Support (ACLS), and the UK Medical Licensing Assessment (PLAB 1 & 2). He has hands-on experience in general medicine, surgery, anaesthesia, ophthalmology, and emergency care. Dr. Petrov has worked in both hospital wards and intensive care units, performing diagnostic and therapeutic procedures, and has contributed to medical education by creating patient-focused health content and teaching clinical skills to junior doctors.

