Can disc prolapse cause weakness in the leg or foot?
A disc prolapse, or slipped disc, is a common spinal condition that can affect more than just your comfort levels. While pain is the most frequent symptom, many individuals in the United Kingdom also experience changes in how their muscles function. When a disc in the lower back presses against a nerve root, it can interrupt the vital electrical signals that tell your leg and foot muscles when and how to move. This resulting weakness is a significant clinical sign that the nerve is under pressure and requires careful monitoring during the recovery process.
What We’ll Discuss in This Article
- How a prolapsed disc interrupts muscle signals
- Recognising the signs of weakness in the leg and foot
- The clinical significance of foot drop
- How healthcare professionals test for muscle strength
- Recovery expectations and the role of physiotherapy
- When muscle weakness becomes a medical emergency
The Connection Between Nerves and Muscles
Every muscle in your leg and foot is controlled by nerves that originate in your spinal cord. These nerves act like electrical cables, carrying messages from your brain to your muscles. In the lumbar spine, these nerve roots pass very close to the intervertebral discs. If a disc prolapses and the inner gel-like material pushes out, it can physically compress the nerve. According to NHS clinical information, this compression can “short-circuit” the signal. When the message to move cannot get through clearly, the muscle becomes weak, even if the muscle tissue itself is perfectly healthy.
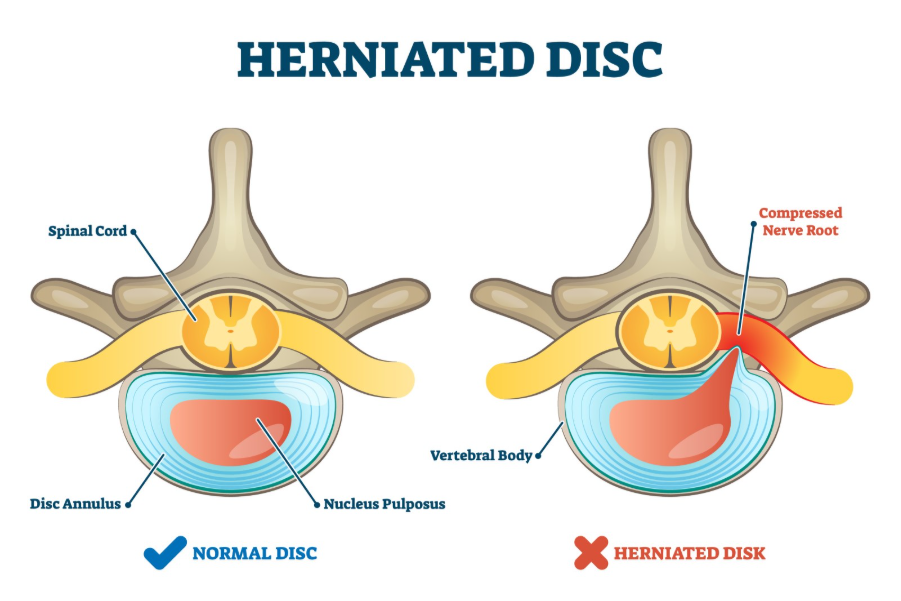
Identifying Weakness in the Leg
Weakness caused by a slipped disc is usually unilateral, meaning it only affects one leg. It may not always feel like a total loss of strength; instead, it might manifest as a feeling of heaviness or a lack of coordination.
- Thigh Weakness: You may find it difficult to climb stairs or get out of a low chair because the muscles at the front of your thigh feel “empty” or unreliable.
- Calf Weakness: It may be difficult to push off the ground when walking or to stand up on your tiptoes.
- Balance Issues: Because the muscles that stabilise your ankle are affected, you might feel less steady on your feet than usual.
Understanding Foot Drop
A specific type of weakness often associated with a slipped disc at the L4 or L5 level of the spine is known as foot drop. This occurs when the muscles responsible for lifting the front part of the foot are weakened. If you have foot drop, you may find that your toes scuff along the ground when you walk, or you might have to lift your knee higher than usual to prevent tripping. NICE guidance identifies persistent or worsening foot drop as a symptom that requires a prompt clinical assessment by a GP or a specialist.
How Muscle Strength is Tested
During a physical examination in the UK, a clinician will perform several tests to grade your muscle strength. They may ask you to walk on your heels and then on your toes to check for subtle signs of weakness. They might also ask you to resist their hand as they push against your foot or big toe. These tests help determine exactly which nerve root in the back is being affected by the prolapsed disc. Comparing the strength of your affected leg to your healthy leg provides a clear baseline to track your recovery over the following weeks.
Recovery and Improving Strength
The good news is that for the majority of patients, muscle strength returns as the pressure on the nerve is relieved. As the body naturally reabsorbs the prolapsed disc material, the “electrical” signal to the muscle is restored.
- Physiotherapy: A physiotherapist can provide specific exercises to keep the muscles active while the nerve heals.
- Nerve Gliding: Exercises designed to gently move the nerve can help reduce the irritation and support the return of normal signaling.
- Activity: Avoiding bed rest is crucial. Gentle walking helps maintain muscle tone and prevents the leg from becoming stiffer.
While pain often settles within 4 to 6 weeks, muscle strength can sometimes take a few months to fully return. Nerves are slow to recover, and patience is a key part of the rehabilitation process.
Conclusion
A disc prolapse can certainly cause weakness in the leg or foot by interrupting the nerve signals from the spine. While this symptom can be concerning, most people in the UK regain their strength through conservative management and staying active. It is a sign that the nerve is under significant pressure and should be monitored by a healthcare professional. If you experience severe, sudden, or worsening weakness, or if you lose control of your bladder or bowels, call 999 immediately.
Is muscle weakness more serious than pain?
Weakness indicates that the motor signals are being blocked, which clinicians usually view as a more significant sign of nerve compression than pain alone.
Can I still walk if my foot feels weak?
If it is safe to do so without tripping, gentle walking is encouraged to keep the muscles functioning and the joints mobile.
Why is only my big toe weak?
Specific nerve roots in the back control specific muscles. Weakness in only the big toe often points to a problem with the L5 nerve root.
Will my leg muscle shrink because of a slipped disc?
If the nerve is compressed for a long time, the muscle can become smaller (atrophy), but this is rare if you stay active and follow a recovery plan.
Does weakness always mean I need surgery?
No, most cases of weakness improve as the disc heals naturally, and surgery is only considered if the weakness is severe or getting worse.
Should I wear a brace for foot drop?
In some cases, a temporary splint called an AFO (Ankle Foot Orthosis) can help you walk safely while waiting for the nerve to recover.
How do I know if the weakness is getting better?
You might notice that you can lift your foot slightly higher or that your leg feels less “heavy” during your daily walk.
Authority Snapshot (E-E-A-T Block)
This article provides an evidence-based explanation of how a disc prolapse can lead to muscle weakness in the lower limbs. The content is written by Dr. Rebecca Fernandez and adheres strictly to the clinical standards provided by the NHS and NICE. Our purpose is to provide accurate, restrained medical education to help UK patients understand their symptoms and recovery path.

