Are there risks of blood clots after leg fractures or immobilisation?
There is a significant and well-documented risk of developing blood clots following a leg fracture or any period of prolonged immobilisation. In the UK, clinicians are particularly vigilant about two related conditions: Deep Vein Thrombosis (DVT), where a clot forms in the deep veins of the leg, and Pulmonary Embolism (PE), which occurs if a piece of that clot breaks off and travels to the lungs. When a leg is fractured or placed in a cast, the natural muscle pump that helps circulate blood back to the heart is deactivated. This leads to blood pooling and a higher likelihood of clot formation. Managing this risk is a critical part of the recovery process for any lower limb injury.
What We’ll Discuss in This Article
- The biology of blood flow: Why immobilisation causes clots
- Identifying the symptoms of Deep Vein Thrombosis (DVT)
- The life threatening risk of Pulmonary Embolism (PE)
- Factors that increase individual risk: Surgery, age, and lifestyle
- UK clinical prevention strategies: Anticoagulants and compression
- When to seek emergency medical attention
Why Immobilisation Increases Clot Risk
Under normal circumstances, every time you walk, your calf muscles contract and squeeze the deep veins, pushing blood upward against gravity.
- Venous Stasis: When a leg is immobilised in a cast or a boot, this pump stops working. The blood flow slows down, a state known as venous stasis.
- Vessel Damage: The trauma of the fracture itself can damage the lining of the blood vessels, which naturally triggers the body’s clotting mechanism as it tries to repair the injury.
- Hypercoagulability: Surgery to fix a fracture can temporarily make the blood stickier as the body responds to the physical stress of the operation.
According to NICE clinical knowledge summaries, the combination of stasis and vessel damage makes leg fractures one of the highest risk factors for venous thromboembolism.
Identifying Deep Vein Thrombosis (DVT)
A DVT usually occurs in the calf or thigh of the injured leg, though it can occasionally happen in the uninjured leg due to general inactivity.
- Swelling: Unexplained swelling in the calf or ankle that feels different from the swelling caused by the fracture itself.
- Pain and Tenderness: A heavy ache or cramping sensation that is often worse when the foot is flexed upward.
- Skin Changes: The skin may feel warm to the touch and appear red or discoloured.
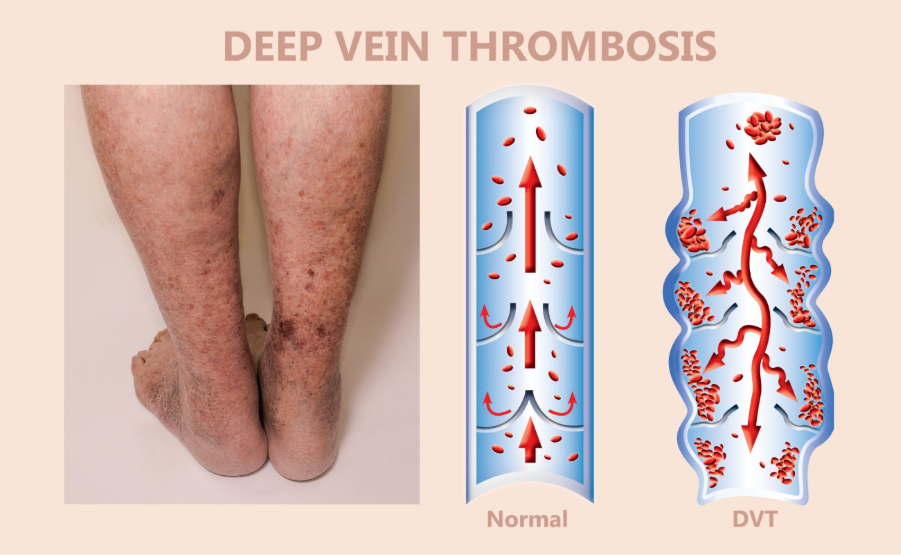
Shutterstock
Explore
The Risk of Pulmonary Embolism (PE)
The most dangerous complication of a DVT is a Pulmonary Embolism. This happens when the clot becomes dislodged and travels through the heart into the arteries of the lungs. This is a medical emergency.
- Warning Signs: Sudden shortness of breath, sharp chest pain that gets worse when breathing deeply, a persistent cough (sometimes with blood), and feeling lightheaded or fainting.
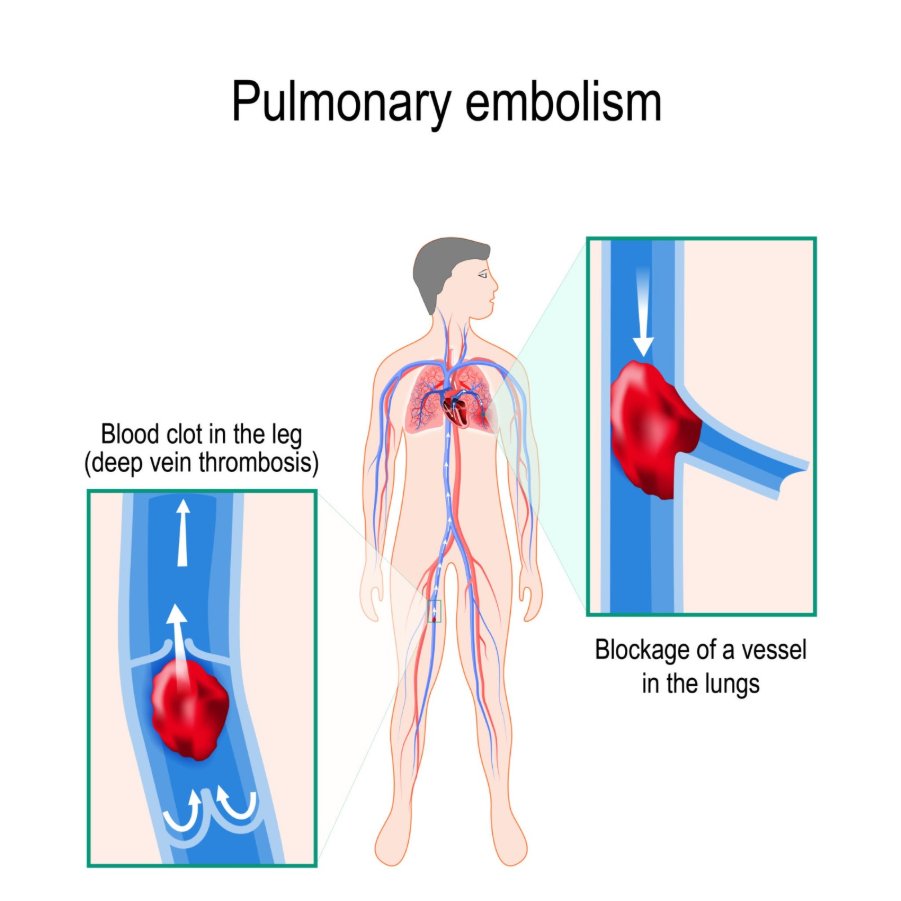
Getty Images
Factors That Increase Your Risk
While anyone with a leg fracture is at risk, certain factors significantly increase the probability of a clot:
- Surgery: Procedures involving plates or screws increase the body’s inflammatory response.
- Location of Fracture: Fractures of the hip, femur (thigh bone), or tibia (shin bone) carry a higher risk than smaller foot fractures.
- Age and Weight: Being over the age of 60 or having a high BMI increases pressure on the venous system.
- Lifestyle and Health: Smoking, pregnancy, or taking the combined oral contraceptive pill can make the blood more prone to clotting.
UK Clinical Prevention Strategies
In the UK, the NHS uses a Risk Assessment for every patient with a lower limb injury to determine the best prevention method:
- Chemical Prophylaxis: You may be prescribed blood-thinning medication (anticoagulants) such as low molecular weight heparin injections or oral tablets for the duration of your immobilisation.
- Mechanical Prevention: The use of anti-embolism stockings or intermittent pneumatic compression devices that mimic the calf pump.
- Early Mobilisation: Moving your toes and performing gentle static muscle squeezes while in the cast to keep the blood moving.
- Hydration: Drinking plenty of water to prevent the blood from becoming too thick.
Conclusion
The risk of blood clots is a serious but manageable part of recovering from a leg fracture. By understanding the link between immobilisation and venous stasis, and by staying vigilant for the symptoms of DVT and PE, you can play an active role in your safety. In the UK, clinicians prioritise the use of preventative medications and early movement to ensure that your recovery from a bone injury is not complicated by a potentially life-threatening clot. If you experience severe, sudden, or worsening symptoms, call 999 immediately.
How long does the risk of a blood clot last?
The risk is highest during the first few weeks of immobilisation, but remains elevated until you are fully mobile and walking normally without a cast or boot.
Can I get a clot in my good leg?
Yes. Because you are less active overall, blood can slow down in both legs. This is why it is important to keep your uninjured leg moving as much as possible.
Do I have to take the injections? I
If a clinician has prescribed anticoagulants, it is essential to take them as directed. They are significantly more effective at preventing clots than aspirin or other over the counter medications.
Can I fly with a leg fracture?
Flying involves long periods of sitting and changes in cabin pressure, which significantly increase the risk of DVT. In the UK, most airlines have strict rules about flying with a cast and may require a Fit to Fly note from your doctor.
Why does my leg swell when I stand up?
Some swelling is normal due to gravity, but if the swelling is persistent, painful, or accompanied by redness, it must be checked to rule out a DVT.
Is it safe to massage my calf if it aches?
No. If you have a clot, massaging the area can dislodge it and cause a pulmonary embolism. If your calf is aching and swollen, seek medical advice first.
What is a D-dimer test?
This is a blood test used by UK doctors to help rule out a clot. It measures a substance that is released when a blood clot breaks up.
Authority Snapshot (E-E-A-T Block)
The purpose of this article is to inform the public about the risks of venous thromboembolism following musculoskeletal injury. The content has been produced by the MyPatientAdvice team and reviewed by Dr. Stefan Petrov, a UK-trained physician with experience in emergency medicine and orthopaedic care. All recommendations are strictly aligned with the current clinical standards of the NHS and NICE.

