Can epidural injections help disc prolapse pain?
Yes, epidural steroid injections (ESIs) are a well established treatment within the NHS for managing the intense leg pain (sciatica) caused by a disc prolapse. While they do not physically “fix” the slipped disc or make it smaller, they are highly effective at reducing the chemical inflammation and swelling around the compressed nerve root. For many patients in the United Kingdom, these injections provide a vital “window of opportunity,” reducing pain enough to allow them to engage with the physiotherapy and movement essential for long-term recovery.
What We’ll Discuss in This Article
- How the injection reduces nerve root inflammation
- The difference between short-term relief and a permanent cure
- The role of fluoroscopy (X-ray guidance) in the procedure
- NHS eligibility criteria and NICE recommendations
- Common side effects versus rare surgical risks
- Integrating injections into a wider rehabilitation plan
How Epidural Injections Work
When a disc prolapses, it doesn’t just physically press on a nerve; it also releases inflammatory chemicals that irritate the nerve fibres. An epidural injection delivers a potent anti-inflammatory (a corticosteroid) directly into the epidural space, the fat-filled area surrounding the spinal cord and nerve roots.
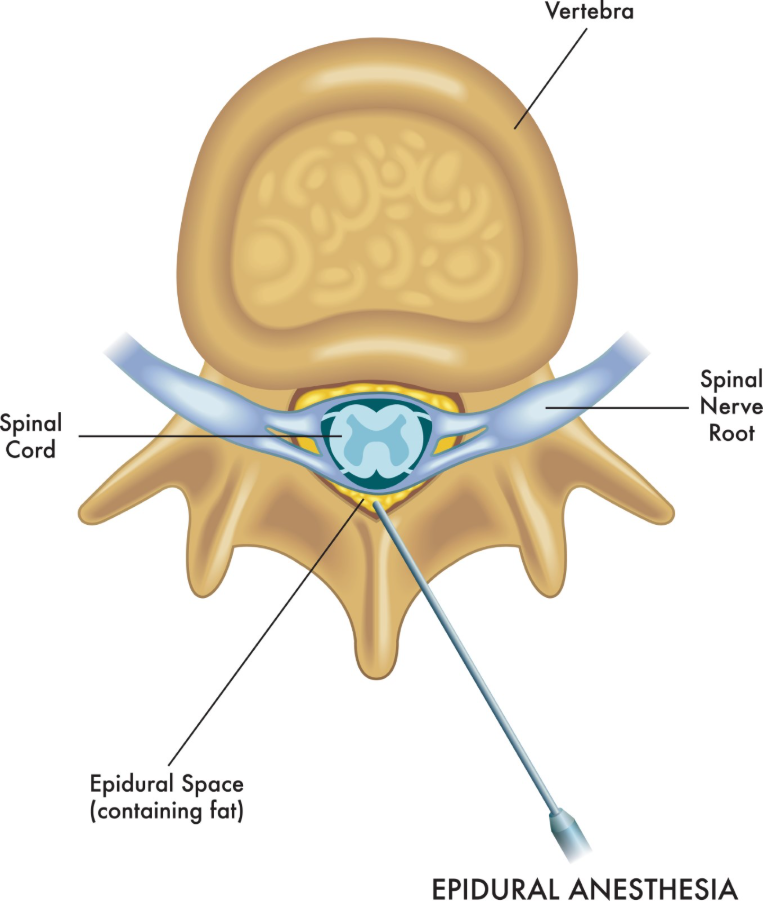
- Reducing Swelling: The steroid “washes away” the inflammatory proteins that cause the nerve to swell and send pain signals.
- Numbing the Area: Most injections also contain a local anaesthetic, which provides immediate, short-term numbing of the affected nerve.
- Breaking the Pain Cycle: By reducing the acute pain, the injection helps relax the secondary muscle spasms that often make back pain worse.
Efficacy and the “Window of Recovery”
According to NICE clinical guidelines, epidural injections are primarily recommended for acute, severe radicular pain (sciatica) rather than general lower back pain.
- Short-Term Relief: Research, including the multicentre NERVES trial, suggests that injections are very effective for short-term relief (typically lasting from a few weeks to several months).
- Success Rates: Approximately 70% to 80% of patients experience significant pain reduction after their first injection.
- Not a Permanent Cure: It is important to remember that the body still needs to reabsorb the prolapsed disc material naturally. The injection simply manages the symptoms while this healing process takes place.
The Procedure: What to Expect
In the UK, these injections are usually performed as a day case in a hospital’s pain clinic or theatre suite.
- Guidance: To ensure safety and accuracy, the NHS recommends that injections are performed under fluoroscopy (live X-ray guidance). This allows the consultant to see exactly where the needle is positioned.
- Positioning: You will usually lie on your front or side. The skin is cleaned, and a local anaesthetic is used to numb the area before the main needle is inserted.
- Contrast Dye: A small amount of dye is often injected first to confirm the medication will spread correctly around the targeted nerve.
- Duration: The procedure typically takes between 15 and 30 minutes, and you will usually be able to go home after a short observation period.
NHS Eligibility and NICE Guidance
The NHS follows strict protocols to ensure injections are offered to those most likely to benefit. You may be eligible if:
- Diagnosis: You have clear radicular pain (sciatica) consistent with a disc prolapse.
- Severity: The pain is having a significant impact on your daily life or ability to work.
- Failed Conservative Care: You have already tried at least 6 to 12 weeks of non-invasive treatments, such as physiotherapy and oral painkillers, without success.
- Age: Typically offered to patients aged 16 and over.
Risks and Side Effects
While epidural injections are generally considered safe, your consultant will discuss potential risks during the consent process.
- Common Side Effects: Temporary soreness at the injection site, a brief “flare-up” of pain for 24 to 48 hours, or temporary numbness/weakness in the legs.
- Dural Puncture: Occasionally, the needle may go slightly too deep, causing a “spinal headache.” This usually settles with rest and fluids but can be quite severe for a few days.
- Rare Complications: Serious issues such as infection, bleeding (haematoma), or permanent nerve damage occur in fewer than 1 in 10,000 cases.
- Steroid Effects: If you are diabetic, the steroid can cause a temporary rise in your blood sugar levels for several days following the injection.
Conclusion
Epidural injections are a powerful tool in the NHS arsenal for managing severe disc prolapse pain. They offer a highly effective way to reduce nerve inflammation and bridge the gap between initial injury and long-term recovery. However, they are most successful when viewed as a facilitator for movement and physiotherapy rather than a standalone cure. If you experience severe, sudden, or worsening symptoms, particularly loss of bladder or bowel control, this is a medical emergency and you should call 999 immediately.
How soon will I feel the benefit?
The local anaesthetic works immediately, but it may wear off after a few hours. The steroid usually takes between 3 and 7 days to start reducing the inflammation and providing more lasting relief.
Can I have the injection if I am taking blood thinners?
You must inform your consultant. Medications like warfarin or clopidogrel may need to be paused for a few days to reduce the risk of bleeding into the spinal canal.
How many injections can I have?
NHS protocols typically limit patients to a maximum of three injections in a 12-month period to minimize the risk of cumulative steroid side effects.
Will I be put to sleep for the procedure?
No, most spinal injections are performed while you are awake so you can provide feedback to the doctor. A light sedative can sometimes be offered if you are particularly anxious.
What if the injection doesn’t work?
If an injection provides no relief, it may suggest that the pain is not coming from that specific nerve root, or that the compression is too severe for anti-inflammatories alone to help. In these cases, a surgical consultation is often the next step.
Can I drive home after the injection?
No, NHS safety rules state you must not drive for 24 hours after the procedure due to the risk of temporary leg weakness or numbness.
Does an epidural help with back pain or just leg pain?
They are significantly more effective for radiating leg pain (sciatica). Their success rate for treating localized “mechanical” lower back pain is much lower.
Authority Snapshot (E-E-A-T Block)
This article examines the clinical efficacy and NHS protocols for epidural injections in treating disc prolapse. The content is written by the MyPatientAdvice Medical Writing/Research Team and reviewed by Dr. Rebecca Fernandez to ensure strict adherence to current NICE and British Pain Society guidelines. Our purpose is to provide balanced, evidence-based education for patients navigating spinal care.

