Can stress trigger fibromyalgia or CFS?
The relationship between stress and the onset of fibromyalgia and chronic fatigue syndrome (ME/CFS) is a central focus of medical research in the UK. While these are distinct biological conditions, clinical evidence and patient histories consistently show that a period of significant stress, whether physical, emotional, or environmental, often acts as a “trigger” that sets the illness in motion. In the UK, the NHS and NICE recognise that stress does not just affect the mind; it has profound effects on the nervous, immune, and endocrine systems. For many people, a major life event or a period of prolonged pressure serves as the tipping point that causes a vulnerable system to transition into a state of chronic illness.
What We’ll Discuss in This Article
- The definition of “trigger events” in chronic illness
- How emotional trauma and life stress impact the nervous system
- The role of physical stress, such as injury or viral infection
- Understanding the “allostatic load” and the tipping point theory
- How ongoing stress can cause symptom flares and relapses
- UK-based strategies for managing the stress-pain cycle
Stress as a biological trigger
In the UK healthcare context, stress is understood as any event that forces the body to adapt. This includes emotional distress, such as a bereavement or a relationship breakdown, but also physical “stressors” like a severe viral infection or a car accident. For many people diagnosed with fibromyalgia or ME/CFS, they can point to a specific window of time where they were under extreme pressure just before their symptoms began.
According to the NHS, fibromyalgia is often triggered by a stressful event. This doesn’t mean stress “causes” the condition in everyone, but in individuals who may have a genetic or biological predisposition, the stress acts as a catalyst. It is thought to “re-wire” the way the central nervous system processes sensory information, leading to the state of central sensitisation, where the body remains in a permanent state of high alert and pain.
For ME/CFS, the trigger is frequently a combination of a viral infection (physical stress) occurring at a time of high emotional or work-related pressure. This “double hit” can overwhelm the body’s ability to recover, leading to systemic energy failure and immune dysfunction characteristic of the condition.
The “Tipping Point” and allostatic load
Medical professionals often use the concept of “allostatic load” to explain why stress triggers these conditions. Allostatic load is the cumulative “wear and tear” on the body that results from being chronically stressed. Think of it like a bucket: your body can handle a certain amount of stress (water) at any one time. However, if you keep adding more stress, work pressure, poor sleep, and emotional worries, without “emptying” the bucket through rest, it eventually overflows.
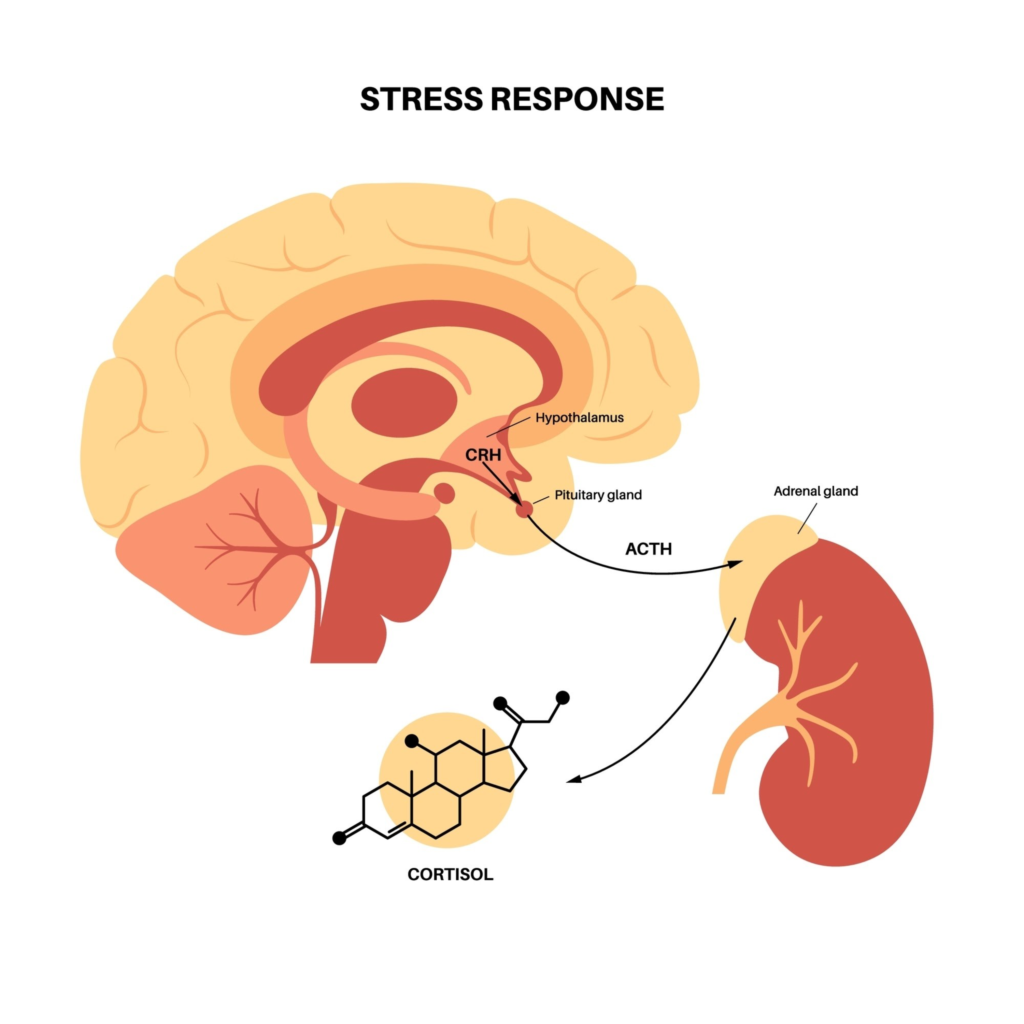
In many patients, the onset of fibromyalgia or ME/CFS represents this overflow or “tipping point.” The body’s regulatory systems, particularly the Hypothalamic-Pituitary-Adrenal (HPA) axis, which manages our stress hormones, effectively break down under the sustained pressure. Instead of returning to a state of calm after a stressful event, the system remains stuck in a dysfunctional “fight or flight” mode.
This theory explains why some people can experience significant stress without getting ill, while others develop a chronic condition. It depends on the individual’s baseline “bucket” size and how many other stressors were already present when the trigger event occurred. Recognising this helps move the conversation away from “it is all in your head” toward an understanding of systemic biological exhaustion.
Physical stress and viral triggers
While emotional stress is a major factor, physical stress is an equally powerful trigger. In the UK, a significant number of ME/CFS cases begin after a severe viral infection, such as Glandular Fever (Epstein-Barr virus) or, more recently, COVID-19. The infection places an enormous metabolic and immune stress on the body. If the individual does not or cannot rest sufficiently during the acute phase, the immune system may fail to “switch off” correctly, leading to chronic post-viral fatigue.
Physical trauma, such as a “whiplash” injury or major surgery, is a frequent trigger for fibromyalgia. The intense pain signals sent to the brain during an injury can, in some cases, cause a permanent change in how the spinal cord filters pain. This is why a person might recover from the initial injury but continue to feel widespread pain in areas that were never actually hurt.
The NICE guidelines for ME/CFS acknowledge that the illness often follows an infection, but they also note that the “trigger” can sometimes be more gradual, such as a slow accumulation of environmental or physical stressors over several years.
Stress and the symptom “flare” cycle
Once a person has developed fibromyalgia or ME/CFS, stress continues to play a major role in the day-to-day management of the condition. In the UK, it is well-recognised that emotional or physical stress is one of the primary triggers for a “flare” or a “crash.” When you are stressed, your body produces chemicals like cortisol and adrenaline, which can increase muscle tension and further sensitise your nerves.
This creates a vicious cycle. The symptoms of the illness, the pain, the fog, and the inability to work, are themselves highly stressful. This stress then triggers further physical symptoms, making the condition harder to manage. Breaking this cycle is a key part of the advice given in NHS pain clinics and fatigue services.
Learning to identify “stress triggers” before they cause a full flare is a vital self-management skill. This might involve recognising that a busy social calendar or a looming deadline at work is starting to push your system too hard. By intervening early with rest and pacing, you can often prevent a minor period of stress from turning into a weeks-long relapse.
Managing the stress-pain connection
Because stress is such a powerful trigger and aggravator, the NHS recommends various strategies to help calm the nervous system. These are not intended to “cure” the condition but to lower the body’s baseline reactivity. Common approaches include:
- Cognitive Behavioural Therapy (CBT): To help manage the emotional burden and anxiety that come with chronic illness.
- Mindfulness and Meditation: Techniques that have been shown to help “down-regulate” the overactive nervous system.
- Pacing: A way of managing physical and mental activity to avoid over-stressing the body’s energy reserves.
- Sleep Hygiene: Ensuring the brain gets the best possible rest to help it process stress more effectively.
UK-based support groups often emphasise that “managing stress” is not about being “perfectly calm,” but about creating a life that respects your new biological limits. Reducing the external pressure you put on yourself, such as letting go of perfectionism or learning to say no to extra commitments, is a practical and effective way to reduce the overall stress load on your system.
Conclusion
Stress, in its various forms, is a significant trigger for the onset of both fibromyalgia and ME/CFS in the UK. Whether it is a sudden physical trauma, a viral infection, or a period of prolonged emotional pressure, stress can act as the catalyst that pushes a vulnerable nervous or immune system into a state of chronic dysfunction. Once the illness is established, stress continues to be a major factor in triggering flares and crashes. By understanding the biological link between stress and these conditions, patients can work with their healthcare providers to implement management strategies that focus on calming the system and protecting their limited energy reserves.
If you experience severe, sudden, or worsening symptoms, call 999 immediately.
Does a stress trigger mean the illness is psychological?
No. Stress causes real, physical changes in the body’s hormones, immune system, and nervous system. The trigger may be emotional, but the resulting condition is a biological reality.
Why did my symptoms start months after the stressful event?
It is common for there to be a delay. The “allostatic load” can build up over time, and the body may only reach its tipping point once the immediate crisis has passed and the system tries to “reset.”
Can reducing stress “cure” my fibromyalgia?
While reducing stress can significantly improve your symptoms and reduce the frequency of flares, it is rarely a “cure” on its own, as the nervous system has already undergone long-term changes.
Is work-related burnout the same as CFS?
No, though they share symptoms. Burnout usually improves with rest and a change in environment, whereas ME/CFS involves a systemic failure where rest does not replenish energy and activity causes a delayed “crash.”
Can positive stress, like a wedding, trigger a flare?
Yes. The body’s stress-response system doesn’t always distinguish between “good” stress (excitement) and “bad” stress (worry). Both require energy and can over-stimulate the nervous system.
How can I tell if a flare is caused by stress or something else?
It is often a combination of factors. Using a symptom diary can help you see if a crash follows a period of high emotional or physical demand.
What is “pacing” in the context of stress?
Pacing involves breaking tasks into small chunks and taking regular rests to ensure you never use up more energy than you have, preventing the physical stress of exhaustion.
Authority Snapshot (E-E-A-T Block)
This article provides a medically accurate overview of the relationship between stress and chronic conditions within the UK. It was prepared by the MyPatientAdvice team and reviewed by Dr. Stefan Petrov to ensure alignment with current NHS and NICE clinical guidance. The purpose of this content is to help patients understand the biological mechanisms of their condition and the importance of holistic management.

