How can pressure sores and joint problems be prevented in non-ambulant patients?
Non-ambulant patients, meaning those who cannot walk and spend the majority of their time in a bed or a chair, face significant risks to their skin and skeletal health. Because these individuals are unable to shift their own weight effectively, prolonged pressure can restrict blood flow to specific areas, leading to tissue death and the formation of painful sores. Similarly, a lack of movement can cause the muscles and tendons around joints to shorten, resulting in permanent stiffness and reduced quality of life. Preventing these complications requires a consistent and structured approach to care that prioritises movement, skin hygiene, and the use of specialist equipment. By following established UK clinical standards, caregivers can protect the physical health and comfort of those with limited mobility.
What We’ll Discuss in This Article
- The clinical importance of regular repositioning and skin checks.
- Using the SSKIN bundle framework for pressure ulcer prevention.
- How range of motion exercises prevent permanent joint contractures.
- Selecting appropriate pressure-relieving mattresses and seating.
- The role of nutrition and hydration in maintaining skin integrity.
- Identifying early warning signs of tissue damage and stiffness.
- When to seek urgent medical assistance for skin or joint issues.
Skin Care and Pressure Sore Prevention
Regular repositioning and skin checks are the primary methods for preventing pressure sores in people with limited mobility. The NHS describes a pressure ulcer as an area of damage to the skin and the tissue underneath it that is caused by a combination of pressure and shear. For non-ambulant patients, repositioning should occur at least every two to four hours, although some individuals may require more frequent changes depending on their skin sensitivity and the surface they are resting on.

Getty Images
The SSKIN bundle is a widely used clinical framework in the UK that helps caregivers remember the essential steps of prevention. This includes Skin inspection, Surface selection, Keep moving, Incontinence management, and Nutrition. Skin inspection should focus on “at-risk” areas where bones are close to the surface, such as the heels, hips, tailbone, and elbows. If an area of skin appears red and does not turn white when pressed, this is a sign of early pressure damage and requires immediate action to remove all pressure from that spot.
Maintaining skin hygiene is also vital. Skin that is frequently damp due to sweat or incontinence is much more likely to break down. Caregivers should use pH-balanced skin cleansers rather than harsh soaps and apply barrier creams where necessary to protect the skin from moisture. However, it is important not to rub or massage reddened areas of skin, as this can cause further damage to the fragile tissues underneath.
Movement and Joint Stiffness Management
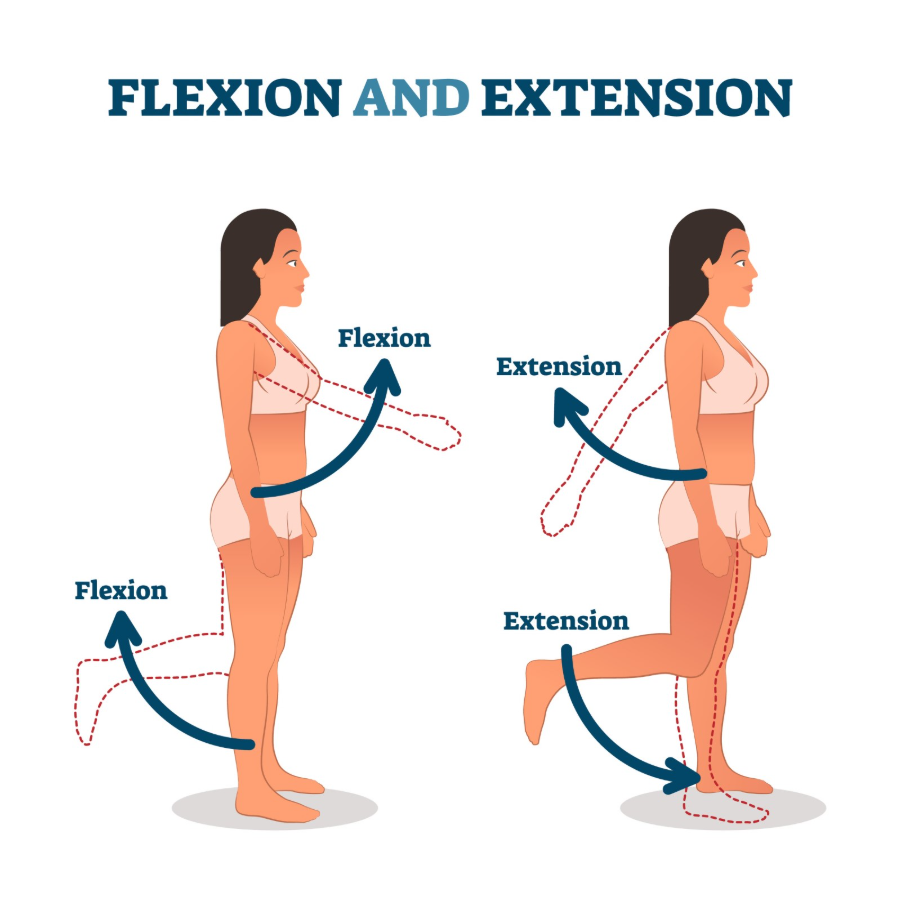
Gentle range of motion exercises and proper positioning are essential to prevent joint stiffness and permanent contractures in non-ambulant patients. A contracture is a permanent shortening of a muscle or joint that often results from a lack of movement in patients with neuromuscular conditions. When a joint remains in one position for a long time, the surrounding connective tissues lose their elasticity, making future movement painful or impossible.
Shutterstock
Range of motion exercises involve gently moving a patient’s limbs through their comfortable extent of movement. These exercises should be performed daily and can often be integrated into routine care, such as during dressing or bathing. Passive stretching, where a caregiver moves the limb for the patient, helps to maintain the length of muscles and tendons. It is crucial to move the joints slowly and stop immediately if the patient shows any signs of pain or resistance.
Positioning aids, such as footboards, hand splints, or specialized pillows, can also help keep joints in a “neutral” position. For example, a pillow placed under the calves can help keep the heels off the bed while also preventing the feet from dropping forward into a position that could cause a permanent tightening of the calf muscles. A physiotherapist can provide a tailored plan that outlines the specific exercises and positions required to protect each joint.
Specialist Equipment and Seating
Specialist pressure relieving equipment such as profiling beds and high specification foam cushions must be used alongside regular movement. NICE clinical guidelines recommend that all people who are assessed as being at risk of developing pressure ulcers should have a documented prevention plan. This plan often includes the provision of “static” or “active” surfaces designed to redistribute weight across a larger area of the body.
Static equipment, such as high-density foam mattresses, works by contouring to the patient’s body shape to reduce pressure on bony prominences. Active or “alternating” equipment uses air cells that automatically inflate and deflate in a sequence, constantly changing the pressure points on the patient’s skin. While these tools are highly effective, they do not replace the need for manual repositioning. They are intended to work in conjunction with regular movement to provide maximum protection.
The following table compares the two primary types of pressure-relieving surfaces used for non-ambulant patients.
| Equipment Type | Mechanism | Best Suited For |
| Static Foam | Contours to the body to spread weight. | Patients at low to medium risk of sores. |
| Alternating Air | Uses moving air cells to shift pressure. | Patients at high risk or with existing sores. |
| Profiling Bed | Adjusts the head and foot height. | Improving posture and easing repositioning. |
| Specialist Seating | Tilt-in-space or custom cushions. | Wheelchair users with limited trunk control. |
| Hybrid Systems | Combines foam with air cells. | Patients who need comfort and high protection. |
Export to Sheets
Nutritional and Hydration Support
Maintaining adequate hydration and balanced nutrition supports skin resilience and helps prevent tissue breakdown. The body requires specific nutrients, particularly protein, vitamins A and C, and zinc, to repair skin cells and maintain the underlying tissues. If a patient is malnourished, their skin becomes thinner and less elastic, making it much more vulnerable to the effects of pressure and friction.
Dehydration is another significant risk factor. When the body is dehydrated, the skin loses its turgor, or plumpness, and becomes more susceptible to “shearing.” Shearing occurs when the skin sticks to a surface while the underlying bone and muscle slide in a different direction, such as when a patient is pulled up in bed. Keeping the skin hydrated from the inside out helps it withstand these mechanical forces.
Caregivers should monitor a patient’s food and fluid intake closely. If a patient has difficulty swallowing or a poor appetite, a referral to a dietitian may be necessary. In some cases, high-protein oral nutritional supplements may be prescribed to ensure the body has the resources it needs to keep the skin healthy. Proper nutrition not only helps prevent sores but also accelerates the healing process if a sore has already begun to form.
Conclusion
Preventing pressure sores and joint problems in non-ambulant patients requires a proactive and consistent care routine focused on skin integrity and movement. By using the SSKIN bundle, performing range of motion exercises, and utilizing specialist equipment, caregivers can significantly reduce the risk of these painful complications. Regular clinical monitoring and adequate nutrition are equally vital in protecting the health of individuals with limited mobility.
If you experience severe, sudden, or worsening symptoms, call 999 immediately.
What is the first sign of a pressure sore?
The first sign is usually a patch of skin that looks red on white skin or purple/blue on darker skin and does not change colour when pressed.
Can a pressure sore happen in just a few hours?
Yes, if a patient is left in one position on a hard surface, significant tissue damage can occur in as little as two hours.
How do I know if a joint is becoming stiff?
You may notice that the joint is harder to move during dressing or that the patient winces when you attempt to move their limb.
Are doughnuts or ring cushions good for pressure relief?
No, ring cushions are not recommended as they can actually restrict blood flow to the centre of the area, making the risk of a sore higher.
Do I still need to move my relative if they have an air mattress?
Yes, while an air mattress helps, regular repositioning is still required to ensure all areas of the skin get a rest from pressure.
What should I do if the skin breaks?
You should contact a healthcare professional, such as a district nurse, immediately to begin a proper dressing and treatment plan.
Does being underweight increase the risk of sores?
Yes, because there is less fat and muscle to act as a “cushion” between the bone and the skin.
Authority Snapshot (E-E-A-T Block)
This guide was developed by the Medical Content Team and reviewed by Dr. Stefan Petrov, a UK-trained physician with experience in general medicine, surgery, and emergency care. The information provided adheres to NHS and NICE standards for the prevention of pressure ulcers and the management of mobility in non-ambulant patients. Our goal is to provide accurate, safe, and factual public health information to support caregivers and patients in the United Kingdom.

