Why does the immune system attack joints in RA or PsA?
Inflammatory arthritis is a complex group of conditions where the body’s natural defence mechanism, the immune system, becomes confused and begins to target healthy tissues. In conditions such as Rheumatoid Arthritis and Psoriatic Arthritis, this internal malfunction leads to persistent inflammation, primarily focused on the joints and surrounding structures. Understanding the biological reasons behind this attack is vital for patients to grasp how their condition progresses and why specific medical treatments are necessary to regulate immune activity.
What We’ll Discuss in This Article
- The fundamental role of the immune system in healthy individuals
- How the body loses the ability to distinguish between self and non-self
- The specific biological mechanism of joint attack in Rheumatoid Arthritis
- The unique pathway of inflammation found in Psoriatic Arthritis
- The role of genetics and environmental triggers in autoimmune responses
- How modern biological therapies aim to correct the immune imbalance
Inflammatory arthritis occurs because the immune system mistakenly identifies the synovium, which is the thin layer of tissue lining the joints, as a foreign invader like a virus or bacteria. This error leads to the recruitment of white blood cells to the joint space, where they release chemicals that cause swelling, pain, and eventual damage to the bone and cartilage. While the exact reason why the immune system turns against the body is still being studied, it is widely accepted that a combination of genetic susceptibility and environmental factors, such as smoking or infection, can trigger this chronic autoimmune response.
The Process of Autoimmune Recognition and Attack
The immune system is a sophisticated network of cells and proteins designed to protect the body from harmful pathogens. In a healthy state, the system can distinguish between the body’s own cells (self) and foreign invaders (non-self). However, in autoimmune conditions like Rheumatoid Arthritis (RA), this distinction breaks down. The immune system begins to produce autoantibodies, which are proteins that specifically target the body’s own tissues.
When these autoantibodies and white blood cells enter the joint, they initiate a cascade of inflammation. This process involves the release of cytokines, which are signalling proteins that tell the body to send more inflammatory cells to the area. This creates a cycle of persistent inflammation that, if left untreated, can lead to the thickening of the joint lining and the destruction of the joint structure.
The Specific Mechanism of Rheumatoid Arthritis
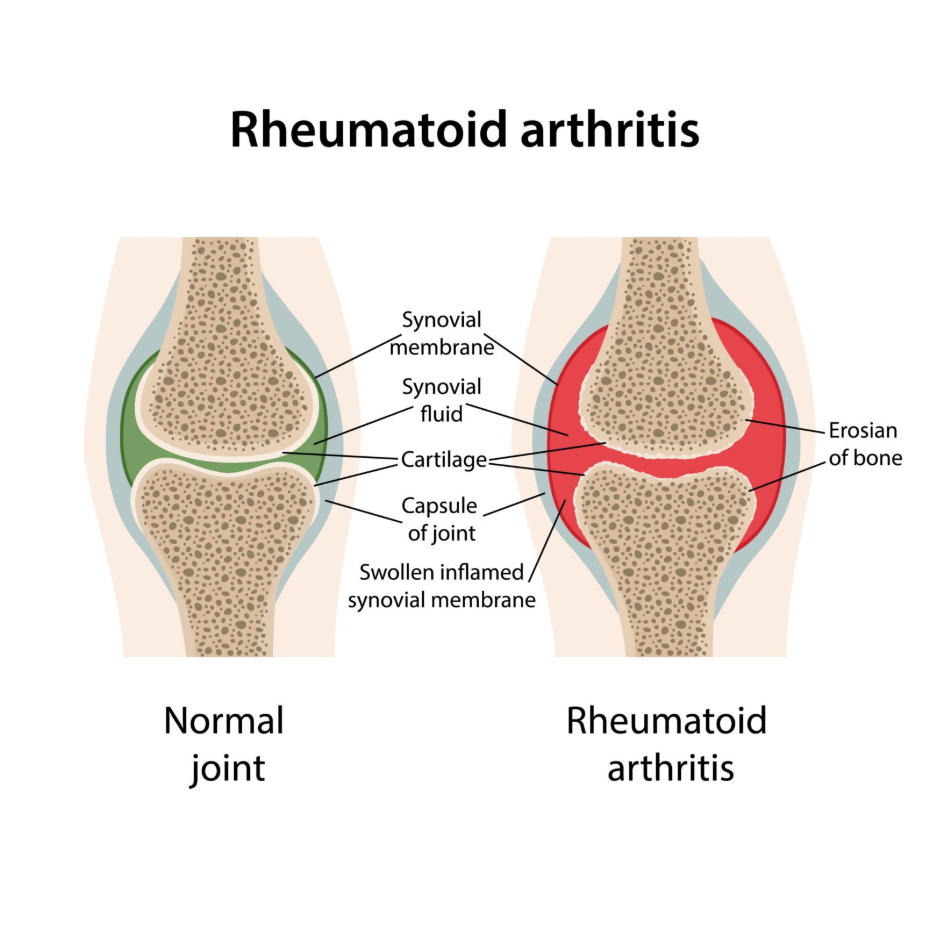
In Rheumatoid Arthritis, the primary site of the immune attack is the synovium. According to the NHS, rheumatoid arthritis is an autoimmune disease where the immune system sends antibodies to the lining of your joints, where they attack the tissue surrounding the joint. This attack causes the synovium to become inflamed and thickened, a state known as synovitis.
As the inflammation persists, the synovium can develop into a layer of rough, granulated tissue called a pannus. This pannus releases enzymes that actively break down the cartilage and bone within the joint. This is why RA often leads to joint deformity and loss of function if the immune response is not brought under control with medication. The attack in RA is typically symmetrical, meaning it affects the same joints on both sides of the body simultaneously.
The Immune Pathway in Psoriatic Arthritis
Psoriatic Arthritis (PsA) shares some similarities with RA, but the immune system often targets different specific structures. While RA focuses heavily on the synovium, PsA frequently involves the enthesis, which is the specific point where a tendon or ligament attaches to the bone. This inflammation is called enthesitis and is a hallmark of the condition.
The NHS describes psoriatic arthritis as a long-term condition that causes joint pain and swelling, and it often occurs in people who have the skin condition psoriasis. The immune system in PsA affects the skin and joints through a shared inflammatory pathway, often involving a specific cytokine called IL-17. This explains why patients with PsA often experience both skin plaques and joint swelling, as the immune system is targeting similar tissues in both locations.
Comparing the Immune Attack in RA vs PsA
While both conditions are autoimmune in nature, the way the immune system behaves and the specific areas it targets can vary significantly.
| Feature | Rheumatoid Arthritis (RA) | Psoriatic Arthritis (PsA) |
| Primary Immune Target | Synovial lining (Synovium) | Enthesis (Tendon to bone junction) |
| Autoantibody Presence | Usually positive for Rheumatoid Factor | Usually seronegative (no autoantibodies) |
| Typical Joint Pattern | Small joints, usually symmetrical | Can affect any joint, often asymmetrical |
| Skin Involvement | Rare, apart from rheumatoid nodules | Very common (Psoriasis) |
| Spine Involvement | Rare, mostly upper neck | Common in some subtypes |
Genetics and Environmental Triggers
The reason the immune system begins this attack is often linked to a person’s genetic makeup. Certain genes, particularly those in the Human Leukocyte Antigen (HLA) complex, are known to increase the risk of developing autoimmune arthritis. These genes help the immune system distinguish the body’s own proteins from those of invaders. If these genes are slightly altered, the system is more likely to make a mistake.
However, genetics alone are usually not enough to cause the condition. Environmental triggers are often required to “switch on” the immune response. Smoking is one of the most significant environmental risks for RA, as it can cause changes in the body that make the immune system more likely to produce autoantibodies. Infections, hormonal changes, and even physical trauma have also been identified as potential triggers that can initiate the first immune attack on the joints.
Conclusion
The immune system attacks the joints in RA and PsA because it incorrectly identifies healthy joint tissues as harmful threats. In Rheumatoid Arthritis, the attack focuses on the synovial lining, while in Psoriatic Arthritis, it frequently targets the points where tendons meet the bone. These complex autoimmune processes are driven by a combination of genetic predisposition and external triggers. Understanding these mechanisms is the foundation for modern treatments that aim to suppress the overactive immune response. If you experience severe, sudden, or worsening symptoms, call 999 immediately.
Why does the immune system only attack certain joints?
The reason why some joints are targeted over others is not fully understood, but it may relate to the amount of mechanical stress a joint faces or the specific proteins present in the tissue of that joint.
Can stress trigger an immune attack on the joints?
While stress does not cause arthritis, high levels of emotional or physical stress can alter immune function and may trigger a flare-up of symptoms in people who already have the condition.
Does an autoimmune attack mean my immune system is weak?
No, in autoimmune arthritis, the immune system is actually overactive rather than weak. It is working too hard, but it is directing its energy toward the wrong targets.
Is it possible to “reset” the immune system?
Currently, there is no way to permanently reset the immune system, but modern medications like biologics can very effectively block the specific parts of the immune system that cause joint damage.
Why are some people “seronegative” if their immune system is attacking them?
Seronegative means the standard autoantibodies are not found in the blood, but the immune system is still causing inflammation through other pathways, such as T-cell activity.
Authority Snapshot (E-E-A-T Block)
This article was created to provide the public with clear, safe, and evidence-based information regarding the autoimmune causes of arthritis. All content is aligned with current NHS and NICE clinical guidance and has been reviewed by Dr. Rebecca Fernandez, a UK-trained physician with extensive experience in internal medicine and emergency care. We aim to support patient understanding of complex biological processes through accurate and transparent medical education.

