Can life-threatening arrhythmias lead to an ICD?
Life-threatening arrhythmias are abnormal heart rhythms that are so severe they can cause the heart to stop pumping blood effectively, leading to sudden cardiac arrest. In the UK, the primary treatment for patients who have experienced or are at high risk of these rhythms is an Implantable Cardioverter Defibrillator (ICD). This device serves as a 24-hour guardian, ready to deliver life-saving therapy the moment a dangerous rhythm is detected.
In this article, you will learn about the specific types of arrhythmias that necessitate an ICD, such as ventricular tachycardia and fibrillation. We will also discuss the underlying causes of electrical instability, common triggers that can set off a cardiac event, and how an ICD provides a level of protection that medication alone cannot achieve.
What We’ll Discuss in This Article
- The definition of life-threatening arrhythmias like VT and VF
- How an ICD identifies and terminates dangerous heart rhythms
- Clinical indications for ICDs in primary and secondary prevention
- Common causes of electrical short-circuits in the heart muscle
- Triggers that can provoke a sudden arrhythmic episode
- Differentiating the functions of an ICD from a standard pacemaker
- Essential emergency guidance for those at risk of cardiac arrest
How life-threatening arrhythmias necessitate an ICD
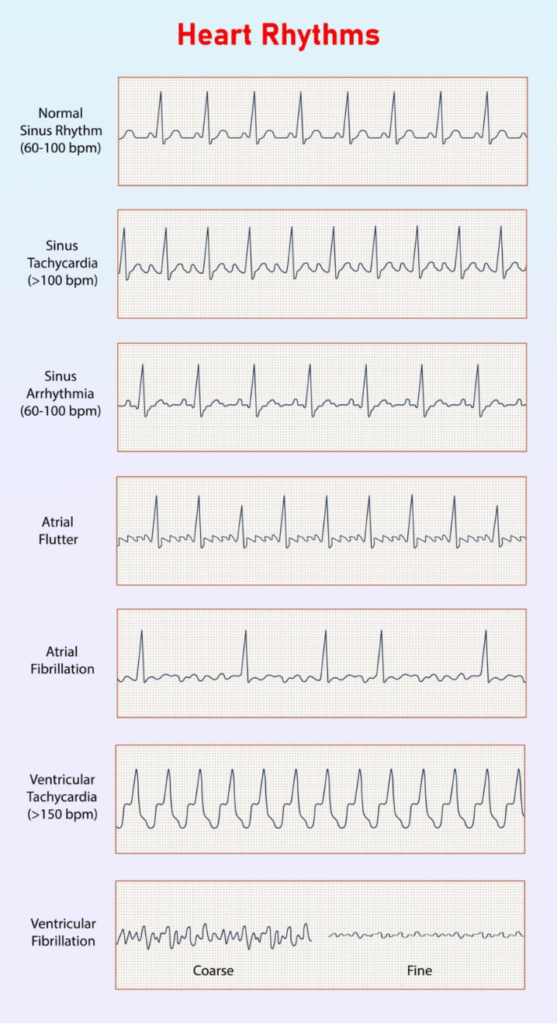
Life-threatening arrhythmias, specifically those originating in the heart’s lower chambers (the ventricles), are the leading cause of sudden cardiac death. When the heart enters a state of ventricular tachycardia (VT) or ventricular fibrillation (VF), the electrical signals become so rapid or chaotic that the heart muscle cannot contract in a coordinated way. Without an immediate electrical shock to reset the rhythm, this condition is fatal within minutes.
An ICD is recommended because it is the only technology capable of delivering a high-energy shock internally and instantly. In the UK, clinicians follow NICE guidelines to identify patients who need this ‘insurance policy.’ This includes individuals who have already survived a cardiac arrest (secondary prevention) and those with specific heart conditions that make a future event statistically likely (primary prevention).
- Ventricular Tachycardia (VT): A very fast but regular heartbeat that can lead to fainting or arrest.
- Ventricular Fibrillation (VF): A chaotic, quivering rhythm that causes immediate collapse.
- Sudden Cardiac Arrest (SCA): The abrupt loss of heart function, breathing, and consciousness.
- Defibrillation: The use of an electrical shock to restore a normal heart rhythm.
Why structural heart disease increases the risk
The relationship between life-threatening arrhythmias and the need for an ICD is often rooted in structural damage to the heart. When the heart muscle is scarred typically due to a previous heart attack the electrical signals cannot pass through the scar tissue. Instead, they may loop around the scar, creating a ‘re-entry’ circuit that triggers a dangerously fast heart rate.
Similarly, conditions that cause the heart muscle to become excessively thick (hypertrophic cardiomyopathy) or stretched and weak (dilated cardiomyopathy) can disrupt the electrical grid. In the UK, a key metric used to decide if an ICD is needed is the ejection fraction (EF). If the heart’s pumping capacity is significantly reduced, the risk of a life-threatening arrhythmia is high enough to justify the implantation of an ICD as a preventative measure.
- Ischaemic Damage: Scarring from a heart attack that disrupts electrical pathways.
- Cardiomyopathy: Diseases of the heart muscle that increase electrical instability.
- Low Ejection Fraction: A measure of heart weakness that correlates with arrhythmia risk.
- Heart Failure: A chronic condition where the heart cannot pump efficiently.
Causes of life-threatening arrhythmias
The underlying causes of life-threatening arrhythmias in the UK are diverse, ranging from lifestyle-related diseases to rare genetic mutations. Coronary artery disease remains the most common cause, as it leads to the heart attacks and scarring mentioned previously. However, not all dangerous rhythms are caused by blockages in the arteries.
Some individuals are born with ‘channelopathies,’ which are genetic defects in the way heart cells handle electrical ions like potassium and sodium. Conditions such as Long QT Syndrome or Brugada Syndrome can cause the heart to suddenly enter a lethal rhythm even if the muscle structure appears normal. Identifying these causes is vital because it helps doctors determine if family members also need to be screened for ICD eligibility.
- Coronary Artery Disease: The primary driver of heart damage in the UK.
- Genetic Syndromes: Inherited conditions that affect the heart’s electrical recovery.
- Heart Valve Disease: Long-term strain from leaky or tight valves that stresses the muscle.
- Myocarditis: Inflammation of the heart muscle, often following a viral infection.
Triggers for sudden arrhythmic events
Even if a person has a known risk of arrhythmias, they may not experience an event until it is ‘triggered’ by an external or internal factor. For patients with certain genetic conditions, a sudden surge in adrenaline caused by intense exercise, a sudden loud noise, or extreme emotional stress can be the trigger that tips the heart into a lethal rhythm.
Other common triggers include severe electrolyte imbalances, such as very low levels of potassium or magnesium, which are necessary for stable heart electricity. In some cases, specific medications (both prescription and over the counter) can prolong the heart’s electrical cycle, acting as a trigger for a dangerous event. This is why patients at risk of life-threatening arrhythmias are often given strict guidance on which medications to avoid.
- Adrenaline Surges: High-intensity sports or sudden emotional shocks.
- Electrolyte Loss: Often caused by severe dehydration or certain diuretic medications.
- Pro-arrhythmic Drugs: Medications that can interfere with heart rhythm stability.
- Alcohol or Stimulants: Excessive intake can destabilise a vulnerable heart.
Differentiation: ICD vs. Pacemaker therapy
It is essential to distinguish between a pacemaker and an ICD, as they address different types of rhythm problems. A pacemaker is used for hearts that are too slow; it provides a gentle, low-voltage nudge to keep the heart beating at a steady rate. Most people with a pacemaker never feel the device working.
An ICD, while it usually includes a pacemaker function, is designed for hearts that go dangerously fast. When it detects a life-threatening arrhythmia, it can first try ‘anti-tachycardia pacing‘ (ATP), which is a series of very fast, painless pulses to ‘break’ the rhythm. If that fails, it delivers a high-voltage shock. This shock is powerful and can be felt by the patient, but it is the definitive therapy that prevents sudden death during a cardiac emergency.
Conclusion
Life-threatening arrhythmias like ventricular tachycardia and fibrillation are the primary reasons why someone would be recommended for an ICD. By detecting these rhythms in seconds and delivering a life-saving shock, the ICD offers a level of protection that medication alone cannot provide. For patients in the UK with heart muscle damage or genetic risks, this device is a critical tool in preventing sudden cardiac arrest and ensuring long-term safety.
If you experience severe, sudden, or worsening symptoms, such as the sensation of a shock followed by dizziness, or if you lose consciousness, call 999 immediately.
Will an ICD stop me from having a heart attack?
No, an ICD manages the electrical rhythm of the heart but does not prevent the arterial blockages that cause a heart attack.
Is the shock from an ICD dangerous?
While the shock can be painful and startling, it is not dangerous; it is a life-saving intervention intended to restart your heart’s normal rhythm.
Can I use a mobile phone with an ICD?
Yes, but you should keep it at least 6 inches (15cm) away from the device and avoid carrying it in a pocket directly over the ICD.
How is the device fitted?
In the UK, it is usually a minor procedure performed under local anaesthetic and sedation, where the device is placed under the skin near the collarbone.
Can I still exercise with an ICD?
Yes, most people can return to exercise, but you should avoid contact sports that could damage the device or its leads.
What happens if the ICD gives me a shock?
You should follow the specific plan provided by your cardiac team, which usually involves contacting your hospital or calling 999.
How long does an ICD battery last?
Typically, the battery lasts between 5 and 9 years, after which the generator is replaced in a simple procedure.
Authority Snapshot
This article was written by Dr. Stefan Petrov, a UK-trained physician with an MBBS and extensive experience in emergency medicine and intensive care. Dr. Petrov has managed acute cardiac emergencies and overseen the care of patients with implanted cardiac devices in hospital settings across the UK. This content follows NHS and NICE safety standards to ensure accurate and evidence-based information for the public.

