How does an ECG help guide device decisions?
The 12 lead electrocardiogram (ECG) is the foundational tool used by UK cardiologists to diagnose electrical failures in the heart. While it is a simple bedside test, the specific patterns it reveals act as a primary map for deciding which cardiac device is most appropriate for a patient. By measuring the timing and path of electrical signals, an ECG distinguishes between a heart that is simply beating too slowly and one that is at risk of dangerous instability.
In this article, you will learn how the waves and intervals on an ECG provide the clinical evidence needed to recommend a pacemaker, an implantable cardioverter defibrillator (ICD), or cardiac resynchronisation therapy (CRT). We will also discuss the importance of QRS duration and how UK clinicians use these metrics to restore a healthy heart rhythm.
What We’ll Discuss in This Article
- Identifying bradycardia and the need for a simple pacemaker
- The role of the PR interval in diagnosing heart block
- How the QRS duration determines the need for CRT devices
- Detecting high risk rhythms that signal the need for an ICD
- Understanding the difference between atrial and ventricular signals
- Using ECG patterns to predict device effectiveness
- Emergency safety guidance for severe rhythm symptoms
Diagnosing the need for a pacemaker
The most common use of an ECG in device decision making is identifying symptomatic bradycardia, which is a heart rate below 60 beats per minute. When an ECG shows long pauses between beats or a consistently slow sinus rhythm that does not speed up with activity, it suggests the heart’s natural timer is failing. This typically leads to a recommendation for a single or dual chamber pacemaker.
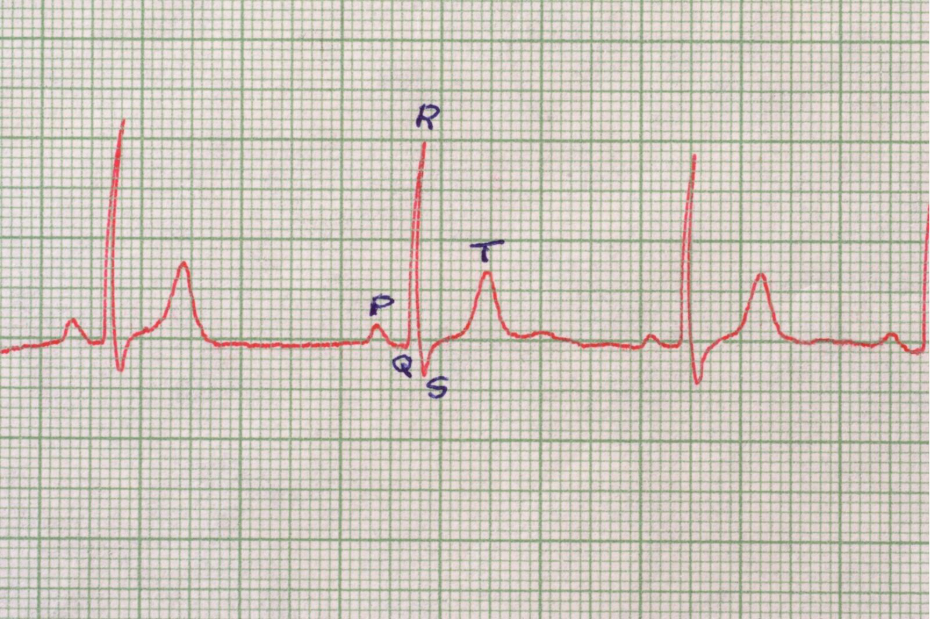
Clinicians also look closely at the PR interval, which measures the time it takes for a signal to travel from the top to the bottom of the heart. If this interval is excessively long or if signals are dropped entirely, the ECG provides the definitive proof required under UK clinical standards to proceed with a pacemaker to bypass the blockage.
- Sinus Bradycardia: A slow rate originating from the heart’s natural pacemaker.
- PR Interval: The time delay between atrial and ventricular contraction.
- Heart Block: Interrupted signals that cause the heart to skip beats.
- Chronotropic Incompetence: A heart rate that fails to rise appropriately during stress.
QRS duration and Cardiac Resynchronisation (CRT)
For patients with heart failure, the QRS complex on an ECG is a critical metric. This part of the trace represents the electrical activation of the ventricles. In a healthy heart, this happens quickly, resulting in a narrow QRS. However, if there is a delay, often caused by Left Bundle Branch Block, the QRS becomes wide. This means the two sides of the heart are beating out of sync.
In the UK, if the QRS duration is measured at 130 milliseconds or more, a specialist device called a CRT is often recommended. This device uses a third lead to pace both ventricles simultaneously, resynchronising the heart’s contraction and significantly improving its pumping efficiency. Without the detailed timing data from the ECG, this life changing therapy could not be accurately prescribed.
- QRS Complex: The electrical signature of the heart’s main pumping chambers.
- Left Bundle Branch Block (LBBB): A specific delay that causes the heart to pump inefficiently.
- Resynchronisation: Using a device to make the heart chambers beat in harmony.
- NICE Criteria: The UK standards that define which QRS widths qualify for CRT.
Screening for ICD eligibility
An ECG is also used to identify patients at high risk of sudden cardiac death who may require an Implantable Cardioverter Defibrillator (ICD). Clinicians look for specific red flag patterns, such as a prolonged QT interval or the characteristic shark fin appearance seen in Brugada syndrome. These patterns indicate that the heart’s electrical system is unstable and prone to lethal, rapid rhythms.
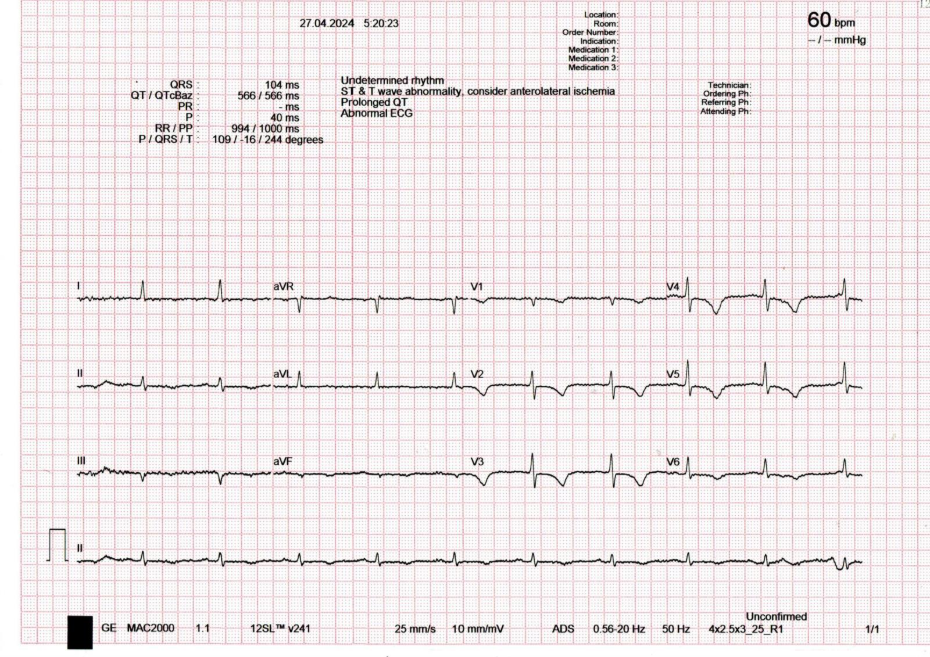
Furthermore, if an ECG or Holter monitor captures episodes of Ventricular Tachycardia (VT), the decision to implant an ICD is often made immediately. In these cases, the ECG serves as the evidence showing that the heart requires a device capable of delivering a life saving shock should a dangerous rhythm recur.
- QT Interval: The time it takes for the heart muscle to electrically reset.
- Ventricular Tachycardia: A life threatening rapid rhythm originating in the ventricles.
- Brugada Syndrome: A genetic condition with a distinct ECG pattern that increases cardiac risk.
- Sudden Cardiac Death Prevention: The primary goal of an ICD device.
Conclusion
The ECG is far more than a simple pulse check; it is a sophisticated diagnostic map that guides almost every device decision in UK cardiology. By revealing the precise nature of electrical delays and instabilities, it allows doctors to choose the specific technology, whether a pacemaker, ICD, or CRT, that will best protect the patient’s heart. For those living with rhythm disorders, the data captured on an ECG is the first and most vital step toward a safer, more active life.
If you experience severe, sudden, or worsening symptoms, such as a sudden blackout, crushing chest pain, or a pulse that feels dangerously slow and irregular, call 999 immediately.
Can an ECG tell if my device battery is low?
While an ECG shows if the device is pacing correctly, a separate device check using a programmer is needed to see the exact battery percentage.
What if my ECG is normal but I still feel like my heart stops?
Rhythm problems can be intermittent. Your doctor may suggest a Holter monitor or an implantable loop recorder to catch symptoms that a standard ECG misses.
Does a wide QRS always mean I need a CRT?
Not necessarily. A wide QRS is one factor; doctors also look at your symptoms and your ejection fraction before deciding.
Is the ECG test painful?
No, it is entirely non invasive. It simply involves placing small sticky pads on your skin to listen to your heart’s electricity.
Can an ECG show if my current pacemaker is failing?
Yes, an ECG can show capture failure or sensing issues, which tell the technician if the pacemaker leads are working as they should.
How long does an ECG take?
The actual recording takes less than a minute, though the setup with the sticky pads takes a few minutes longer.
Do I need an ECG before every cardiology appointment?
Often, yes. It provides your doctor with a current baseline to see if your rhythm has changed since your last visit.
Authority Snapshot
This article was written by Dr. Rebecca Fernandez, a UK trained physician with an MBBS and extensive experience in cardiology and internal medicine. Having managed acute rhythm emergencies and supervised cardiac monitoring in NHS hospitals, Dr. Fernandez provides expert insight into how diagnostic data translates into life saving device therapy. This content adheres to current UK clinical guidelines to ensure public health accuracy.

