What tests confirm the need for a pacemaker?
A pacemaker is recommended when diagnostic tests confirm that the heart’s natural electrical system is failing to maintain a safe or effective heart rate. In the UK, the clinical decision to implant a pacemaker follows a specific pathway aimed at correlating a patient’s symptoms (such as fainting or dizziness) with documented evidence of a slow or irregular heart rhythm.
In this article, you will learn about the primary diagnostic tools used by cardiologists, ranging from simple bedside tests like the ECG to advanced long-term monitoring solutions. We will also discuss the role of exercise testing and electrophysiology studies in confirming complex rhythm disorders.
What We’ll Discuss in This Article
- The role of the 12 lead ECG in capturing immediate rhythm problems
- Why ambulatory monitoring (Holter monitors) is used for intermittent symptoms
- The use of event recorders and implantable loop recorders for rare episodes
- How exercise stress tests evaluate the heart’s response to physical demand
- The clinical purpose of an electrophysiology (EP) study
- The importance of the Tilt Table test for unexplained fainting
- UK clinical standards for diagnosing heart block and sick sinus syndrome
The Initial Step: 12 Lead ECG
The first and most essential test is the 12 lead electrocardiogram (ECG). This simple, non-invasive test records the electrical activity of your heart over a few seconds using stickers placed on your chest, arms, and legs. It provides a “snapshot” of your heart rhythm and can immediately identify persistent issues such as third-degree heart block or severe sinus bradycardia.
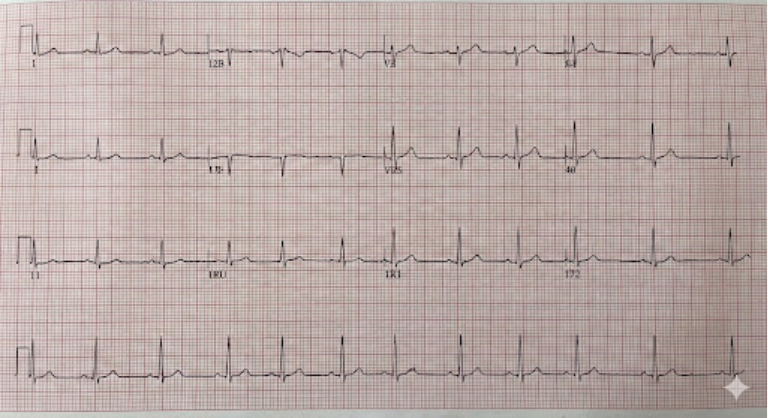
However, many heart rhythm problems are intermittent, meaning they may not happen during the short window of a standard ECG. If the ECG appears normal but your symptoms persist, UK clinicians will move to more advanced monitoring techniques to “catch” the rhythm abnormality when it occurs.
- ECG Snapshot: Captures immediate, persistent rhythm failures.
- Heart Block Detection: Identifies delays or blocks in the AV node.
- Sinus Node Function: Evaluates the health of the heart’s natural pacemaker.
- Baseline Data: Provides a comparison for future tests.
Ambulatory Monitoring (Holter Monitor)
If your symptoms happen daily or every few days, you may be asked to wear a Holter monitor. This is a small, portable ECG device that you wear for 24 to 48 hours (and sometimes up to a week). It records every single heartbeat during that period while you go about your normal daily activities.
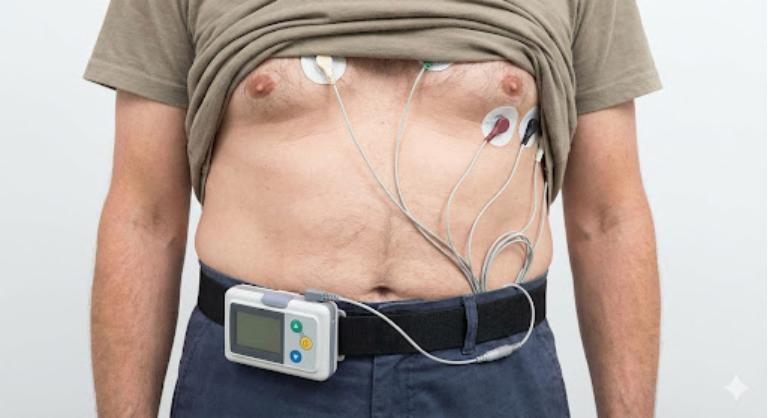
The goal of a Holter monitor is to correlate your symptoms with your heart rhythm. If you feel dizzy at 2:00 PM and the monitor shows your heart rate dropped to 30 beats per minute at exactly that time, this “correlation” is often the definitive evidence needed to confirm that a pacemaker is required.
- Continuous Recording: Monitors every heartbeat over 24 or 48 hours.
- Symptom Diary: Patients record when they feel unwell to match with the heart trace.
- Intermittent Capture: Effective for symptoms that occur frequently.
- Non-Invasive: Small and lightweight, allowing for normal activity.
Long Term Monitoring: Loop Recorders
For patients whose symptoms are rare, happening once a month or once a year, short-term monitors are often insufficient. In these cases, a cardiologist may recommend an Implantable Loop Recorder (ILR). This is a tiny device, about the size of half an ice-lolly stick, that is inserted just under the skin of the chest during a minor procedure.
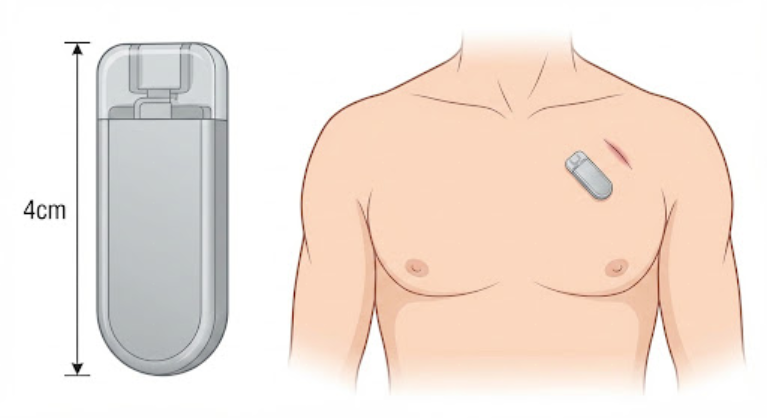
The ILR can monitor the heart for up to three years. It automatically records very slow or very fast rhythms and can also be “triggered” by the patient using a handheld remote when they feel a symptom. Because it provides such a long-term safety net, it is highly effective at diagnosing the cause of infrequent blackouts (syncope) that other tests have missed.
- ILR: A long-term implantable device for rare, unexplained symptoms.
- Automatic Recording: Captures events even if the patient is unconscious.
- Patient Trigger: Allows the user to flag symptoms manually.
- Diagnostic Gold Standard: Often the final step for complex fainting cases.
Exercise Stress Testing
Sometimes, a heart rhythm is normal at rest but fails to speed up appropriately during physical activity. This is known as “chronotropic incompetence.” To test for this, you may undergo an exercise stress test, usually on a treadmill or stationary bike, while connected to an ECG monitor.
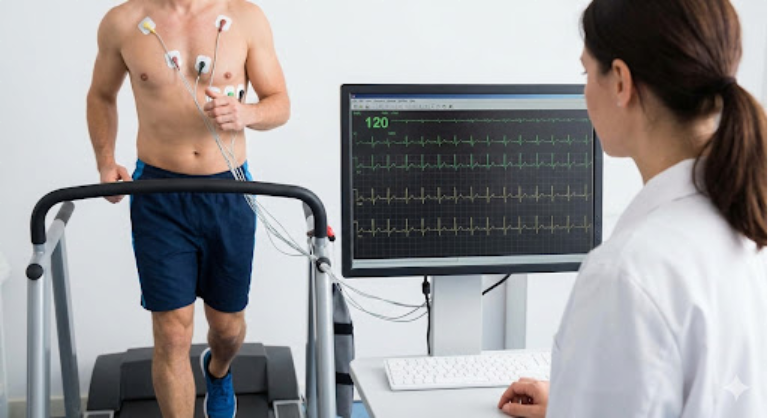
In the UK, this test helps determine if a pacemaker with “rate-responsive” features is needed. If the heart rate remains slow despite intense exercise, or if a specific type of heart block is triggered by exertion, a pacemaker becomes a necessary intervention to allow the patient to remain active and safe.
- Exertional Monitoring: Evaluates the heart’s electrical response to stress.
- Rate Response: Determines if the heart can meet physical demands.
- Provocation Test: Sometimes unmasks blocks that are hidden at rest.
- Safety Protocol: Performed under medical supervision in a hospital.
Electrophysiology (EP) Study
An EP study is a more invasive test used when other diagnostic methods have failed to provide a clear answer. During this procedure, thin, flexible wires are threaded through a vein in the groin up into the heart. These wires can record electrical signals from inside the heart chambers with extreme precision.
The cardiologist can use these wires to “map” the heart’s electrical system and even try to provoke an abnormal rhythm in a controlled environment. This test is highly accurate at identifying exactly where the electrical system is failing, providing definitive confirmation for a pacemaker or ICD implantation.
- Invasive Mapping: Records signals directly from inside the heart muscle.
- Provocative Pacing: Testing how the heart reacts to different electrical speeds.
- Precise Diagnosis: Identifies the exact location of electrical blocks.
- Clinical Insight: Helps choose the best type of device for the patient.
Conclusion
Confirming the need for a pacemaker involves a logical clinical progression from non-invasive snapshots like the ECG to long-term monitoring or invasive mapping. Each test aims to prove that a slow or irregular heart rhythm is the direct cause of a patient’s symptoms. By using these diagnostic tools according to UK safety standards, cardiologists can ensure that a pacemaker is only fitted when it will provide a clear benefit to the patient’s health and safety.
If you experience severe, sudden, or worsening symptoms, such as a sudden blackout, crushing chest pain, or a pulse that feels dangerously slow and irregular, call 999 immediately.
Can a single ECG prove I need a pacemaker?
Yes, if it shows a high-grade heart block or a dangerous pause, an ECG can be enough to justify immediate implantation.
What if all my tests come back normal but I still feel dizzy?
In this case, your doctor might recommend a long-term monitor like an implantable loop recorder to wait for a symptomatic event.
Is an EP study dangerous?
It is an invasive procedure and carries small risks like bleeding or bruising, but it is considered very safe and provides vital information.
How long does a Holter monitor take to get results?
Once you return the device, the data is analysed by a cardiac physiologist, which usually takes a few days.
Can I shower while wearing a Holter monitor?
Most standard Holter monitors are not waterproof and must be kept dry, but your clinic will give you specific instructions.
Do I need a pacemaker for a heart rate of 55?
Not necessarily; many healthy people (and athletes) have a resting rate of 50 to 60. It only requires a pacemaker if it causes symptoms.
What is a Tilt Table test?
It is a test used to see if changes in posture trigger fainting, helping to distinguish between heart problems and simple faints.
Authority Snapshot
This article was written by Dr. Rebecca Fernandez, a UK-trained physician with an MBBS and extensive experience in cardiology and internal medicine. Having performed diagnostic assessments and managed cardiac cases in the NHS, Dr. Fernandez provides expert insight into the clinical pathways for rhythm diagnosis. This content follows NHS and NICE safety standards to ensure accurate heart health information.

