What symptoms of coronary artery disease or heart attack in people with diabetes or older adults might be easy to miss?
We are often taught that a heart attack feels like a crushing weight on the chest. However, for two specific groups, older adults and people with diabetes, this classic warning sign is frequently absent. Instead, heart problems may manifest as vague symptoms like sudden tiredness, mild breathlessness, or even confusion. Because these signs are easily mistaken for the flu, indigestion, or general aging, diagnosis is often delayed, leading to poorer outcomes. Recognising these ‘silent’ symptoms is a vital skill for patients and caregivers alike.
What We’ll Discuss in This Article
- Why diabetes and aging change the way heart attack symptoms feel.
- The specific ‘silent’ symptoms like breathlessness and confusion.
- The role of diabetic neuropathy in masking chest pain.
- How symptoms differ from the classic ‘Hollywood heart attack.’
- The danger of attributing symptoms to ‘just getting older.’
- Physiological reasons for these differences (autonomic dysfunction).
- When to seek emergency help for vague symptoms.
What symptoms are easy to miss in these groups?
In older adults and people with diabetes, the most common missed symptoms of a heart attack include sudden shortness of breath without chest pain, profound unexplained fatigue, nausea (often mistaken for a stomach bug), and sudden confusion or delirium. Instead of pain, the body may signal distress through a sudden drop in blood pressure (fainting) or excessive sweating.
The ‘Silent’ Presentation
- Breathlessness (Dyspnoea): This is often the only symptom. A patient may suddenly feel winded while sitting still or walking a short distance.
- Fatigue: A deep, sudden exhaustion that is disproportionate to activity.
- Delirium: In the elderly, a sudden change in mental state (confusion, agitation) is a common sign of physical illness, including heart attacks, as reduced blood flow affects the brain.
- Syncope (Fainting): A sudden collapse without warning can be the first sign of a cardiac event in these groups.
Why do people with diabetes often lack chest pain?
People with diabetes are at high risk of ‘silent myocardial infarction’ due to cardiac autonomic neuropathy, according to an article published by Healthline (July 2025). High blood sugar levels over time damage the nerves that transmit pain signals from the heart to the brain. Consequently, even during a severe heart attack, the patient may feel no chest pain at all, or only mild discomfort that they dismiss as indigestion.
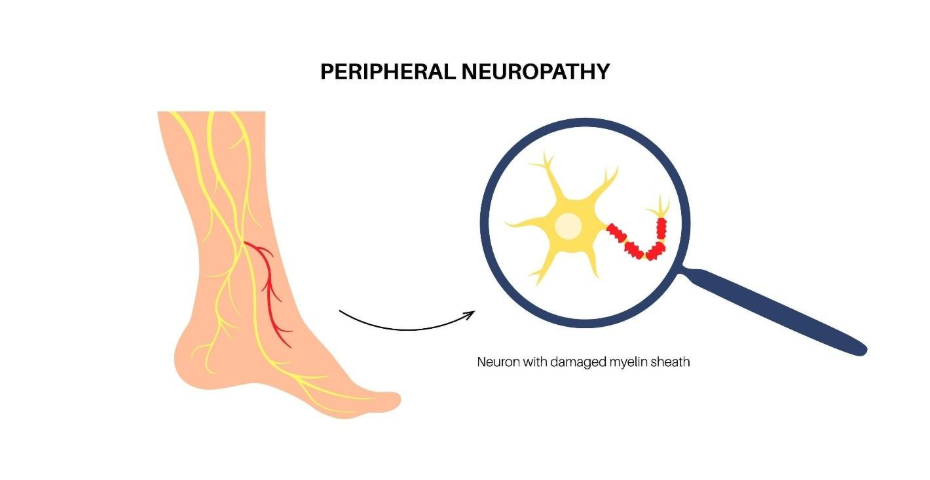
Shutterstock
The Mechanism of Neuropathy
The heart has a network of nerves that act as an alarm system.
-
Damage: Diabetes damages the myelin sheath protecting these nerves.
- Signal Failure: When the heart muscle is starved of oxygen (ischaemia), the ‘pain’ signal is sent but never reaches the brain effectively.
- Autonomic Symptoms: Because the pain pathway is blocked, the body uses other pathways, triggering sweating (diaphoresis) or nausea via the vagus nerve instead.
Why do older adults present differently?
Aging affects the body’s sensitivity to pain and alters the physiological response to stress. Older adults are more likely to have ‘collateral circulation’ (extra blood vessels that develop over time), which may change how pain is felt. Additionally, the presence of other conditions (comorbidities) like arthritis or dementia can mask or complicate the recognition of heart symptoms.
- Altered Pain Perception: Pain thresholds increase with age, meaning a stimulus that would hurt a younger person might not register as sharply.
- Comorbidities: An older adult with chronic back pain or arthritis might ignore cardiac back or arm pain, assuming it is just a flare-up of their existing condition.
- Cognitive Decline: Patients with dementia may be unable to articulate that they are in pain, expressing it instead through agitation or withdrawal.
Common Triggers for Silent Attacks
In these vulnerable groups, heart attacks can be triggered by physical stress (like an infection) or environmental factors rather than just exercise. A bout of the flu, a urinary tract infection (UTI), or a sudden cold snap can place enough strain on the heart to trigger an event that presents purely as a worsening of their general condition.
- Infections: Pneumonia or flu increases the heart’s metabolic demand, tipping a stable blockage into a heart attack.
- Post-Prandial Hypotension: A drop in blood pressure after eating can trigger cardiac ischaemia in the elderly.
- Dehydration: Older adults are prone to dehydration, which thickens the blood and increases clot risk.
Differentiating ‘Old Age’ vs. Medical Emergency
It is dangerous to assume that slowing down or feeling tired is ‘just old age.’ The key differentiator is the speed of onset. Aging is gradual; a heart attack is acute. If an older person who was walking fine yesterday is suddenly too breathless to cross the room today, this is a medical red flag, not natural aging.
Comparison Table: Aging vs. Acute Event
| Feature | Normal Aging / Chronic Issue | Potential Silent Heart Attack |
| Onset | Gradual (weeks/months) | Sudden (hours/minutes) |
| Fatigue | Tired at the end of the day | Exhausted after minor effort |
| Confusion | Slow cognitive decline | Sudden delirium or confusion |
| Breathing | Breathless after heavy exertion | Breathless at rest or light activity |
| Digestion | Chronic reflux after spicy food | Sudden nausea/vomiting without cause |
Conclusion
For people with diabetes and older adults, the absence of chest pain does not mean the absence of a heart attack. Symptoms like sudden breathlessness, confusion, fainting, or ‘flu-like’ fatigue are serious warning signs that require immediate assessment. Recognising that these groups have a different biological ‘alarm system’ is crucial for ensuring they receive life-saving treatment in time.
If an older adult or person with diabetes experiences sudden shortness of breath, confusion, fainting, or profuse sweating, even without chest pain, call 999 immediately.
Can a blood sugar drop feel like a heart attack?
Yes. Hypoglycaemia (low blood sugar) causes sweating, palpitations, confusion, and dizziness, mimicking a heart attack. A quick blood sugar test is essential to rule this out.
Is shoulder pain common in the elderly during a heart attack?
Yes. Older adults often complain of vague aching in the shoulders, neck, or jaw rather than central chest pain.
Why is confusion a heart symptom?
The brain is extremely sensitive to oxygen levels. If the heart is not pumping effectively (due to an attack), the brain gets less oxygen, leading to acute confusion or delirium.
Should diabetics have regular heart screenings?
Yes. Because symptoms are often silent, regular check-ups (checking blood pressure, cholesterol, and kidney function) are vital. Some doctors may recommend periodic stress tests.
What is ‘atypical’ angina?
This refers to angina symptoms that don’t fit the classic profile, such as abdominal pain, breathlessness, or stabbing pain, which are more common in these high-risk groups.
Does dementia affect heart attack diagnosis?
Yes. Patients with dementia may not be able to report symptoms. Caregivers should look for non-verbal signs like grimacing, rubbing the chest, or sudden behavioural changes.
Can a fall be a sign of a heart attack?
Yes. In older adults, a ‘drop attack’ or unexplained fall can be caused by the sudden drop in blood pressure or arrhythmia associated with a heart attack.
Authority Snapshot
This evidence-based guide adheres strictly to NHS guidelines on Coronary heart disease and NICE clinical guidelines, providing clear, safe, and factual information on the definition and impact of coronary artery disease. The content has been authored and reviewed by professionals, including Dr. Rebecca Fernandez, a UK-trained physician with extensive experience in cardiology and emergency medicine. This article explains the causes of heart ischaemia, reinforces safety protocols, and does not offer diagnostic advice, ensuring readers receive accurate, trustworthy public health information.

