Can High Blood Pressure Make Me Feel Anxious or Restless?
The relationship between our physical health and our emotions is deeply intertwined. Many people find that when they feel anxious or restless, their heart races and they worry that their blood pressure has reached a dangerous level. Conversely, those diagnosed with hypertension often wonder if the condition itself is the source of their jittery or uneasy feelings. Because the body uses the same biological ‘alarm system’ for both stress and cardiovascular regulation, it can be difficult to tell which came first. This article explores the science behind these sensations, clarifying what is a symptom, what is a side effect, and what is simply a normal response to life’s pressures.
What We’ll Discuss in This Article
- The physiological relationship between blood pressure spikes and feelings of anxiety.
- Why high blood pressure is usually ‘silent’ but can mimic physical signs of stress.
- The ‘feedback loop’ where anxiety raises blood pressure and vice versa.
- Common lifestyle causes that contribute to both hypertension and restlessness.
- Environmental triggers like caffeine and nicotine that influence your mood and heart.
- The difference between primary hypertension and secondary causes of restlessness.
- When to use specific mental health screening tools for monitoring.
The Connection Between Blood Pressure and Feelings of Anxiety
High blood pressure does not typically cause feelings of anxiety or restlessness directly. For most people, hypertension is ‘silent’ and produces no physical sensations. However, a sudden spike in blood pressure known as a hypertensive crisis can trigger a surge of adrenaline that makes you feel intensely anxious, restless, or panicked. More commonly, it is the anxiety itself that causes a temporary rise in blood pressure.
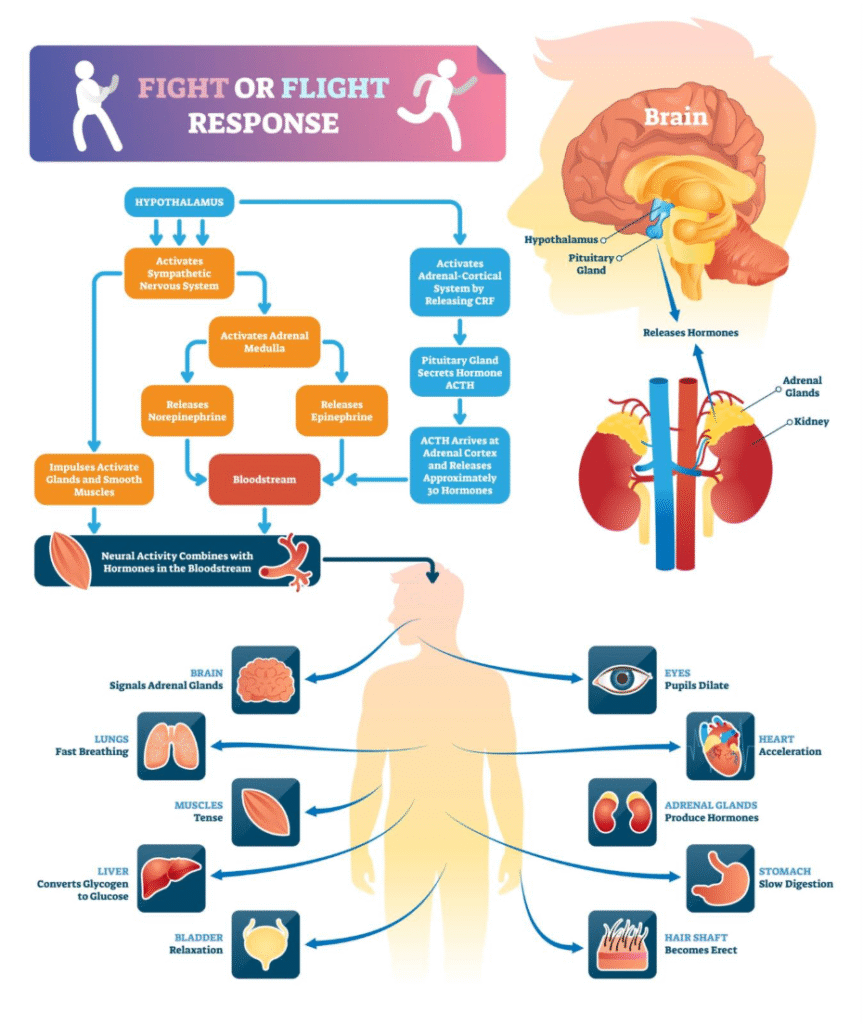
In the UK, the NHS notes that while the two conditions often occur together, they are usually separate issues. When you are anxious, your body releases hormones like cortisol and adrenaline. These hormones make your heartbeat faster and narrow your blood vessels, which naturally causes a temporary increase in blood pressure. If you are already prone to hypertension, this can lead to a cycle where the physical sensation of a racing heart makes you feel even more restless, creating a challenging feedback loop.
The ‘Feedback Loop’ of Anxiety and Hypertension
The link between anxiety and high blood pressure is often described as a cyclical relationship. While anxiety doesn’t cause long-term, chronic hypertension on its own, frequent bouts of anxiety can lead to repeated blood pressure spikes. Over time, these spikes can damage your blood vessels, heart, and kidneys, just as chronic high blood pressure would.
This loop often manifests in several ways:
- White Coat Effect: Feeling anxious in a medical setting causes a high reading, which then increases the patient’s anxiety about their health.
- Hypervigilance: Constantly checking your blood pressure at home can lead to ‘monitor-induced anxiety,’ where the stress of testing causes the numbers to rise.
- Physical Mimicry: A temporary spike in pressure (due to exertion or caffeine) may cause a slight thumping in the chest, which an anxious person may misinterpret as a panic attack.
Causes of Anxiety and High Blood Pressure
The causes of both high blood pressure and anxiety are frequently rooted in the same lifestyle and biological factors. In the UK, medical professionals look at these ‘shared risk factors’ to treat the patient, rather than just treating the numbers on a blood pressure cuff.
Common shared causes include:
- Chronic Stress: Long-term pressure at work or home keeps the body in a state of high alert, raising both anxiety levels and baseline blood pressure.
- Poor Sleep Quality: Conditions like sleep apnoea cause restlessness at night and are a major driver of daytime hypertension.
- Sedentary Lifestyle: A lack of physical activity reduces the body’s ability to ‘burn off’ stress hormones, leading to both a higher resting heart rate and increased restlessness.
- Genetics: Some people are biologically more sensitive to the effects of stress hormones, making them more likely to experience both mood and pressure fluctuations.
Triggers for Restlessness and Pressure Spikes
Certain daily triggers can simultaneously cause your blood pressure to rise and make you feel jittery or restless. These triggers stimulate the nervous system directly, often mimicking the symptoms of a panic attack. Identifying these triggers is a key step in managing both your cardiovascular health and your mental well-being.
Frequent triggers include:
- Excessive Caffeine: High doses of coffee or energy drinks stimulate the heart and can cause ‘caffeine jitters’ that feel identical to anxiety.
- Nicotine: Smoking or vaping causes an immediate spike in blood pressure and acts as a stimulant that can increase restlessness.
- Alcohol Withdrawal: Even mild ‘hangovers’ involve a period where the body is in a hyper-excited state, leading to higher blood pressure and ‘the shakes.’
- Specific Medications: Some decongestants or asthma treatments can cause a racing heart and feelings of unease as a side effect.
Primary vs. Secondary Causes of Restlessness
In clinical practice, it is important to distinguish between primary anxiety (a mood disorder) and restlessness caused by a secondary medical condition. Some secondary causes of high blood pressure are famous for producing intense physical symptoms that feel exactly like a panic attack.
| Feature | Primary Anxiety / Hypertension | Secondary (Medical Cause) |
| Example | Lifestyle/Genetics/Stress | Overactive Thyroid or Adrenal Issue |
| Feelings | General worry or dread | Intense physical jitters, sweating, palpitations |
| BP Pattern | Spikes during stressful moments | Can be high even when feeling calm |
| Diagnosis | Clinical monitoring and history | Blood tests and imaging (e.g., thyroid tests) |
For example, an overactive thyroid (hyperthyroidism) can make a person feel incredibly restless and anxious while also driving their blood pressure higher.
Conclusion
While high blood pressure is usually silent, the physical sensations of anxiety and restlessness are often closely linked to how our heart and blood vessels react to stress. Understanding that your feelings of unease may be driving your numbers rather than the other way around can help you manage your health more effectively. By addressing both your mental well-being and your physical habits, you can break the feedback loop and support a healthier cardiovascular system.
If you experience severe, sudden, or worsening symptoms such as chest pain, a sudden change in vision, or a severe headache, call 999 immediately.
You may find our free Anxiety Test helpful for understanding or monitoring your symptoms.
Can a panic attack cause a stroke?
While a panic attack causes a temporary spike in blood pressure, it rarely causes a stroke in a healthy person; however, chronic stress should be managed to protect long-term health.
Why do I feel restless after taking blood pressure medication?
Some medications can cause side effects like a cough or mild dizziness that might make you feel uneasy; discuss any persistent restlessness with your GP.
Does deep breathing lower blood pressure?
Yes, deep, slow breathing activates the parasympathetic nervous system, which can help lower your heart rate and blood pressure in the short term.
Can high blood pressure cause ‘brain fog’?
Is my anxiety making my blood pressure medication less effective?
Unmanaged chronic anxiety can keep your blood pressure higher than it should be, making it harder for your medication to reach your target numbers.
How can I tell the difference between anxiety and a heart problem?
It can be difficult; however, heart-related chest pain usually feels like ‘pressure’ and worsens with exercise, whereas anxiety often occurs at rest.
Authority Snapshot
This article has been reviewed by Dr. Rebecca Fernandez, a UK-trained physician with an MBBS and extensive experience in cardiology, internal medicine, and psychiatry. Dr. Fernandez has a unique background in managing both acute physical emergencies and mood disorders, ensuring this guide provides a balanced, evidence-based view of the link between cardiovascular health and mental well-being. Following NHS and NICE protocols, this article explores how blood pressure and anxiety intersect and when to seek professional help.

