Does Rheumatic Fever Still Cause Valve Problems?
While rheumatic fever is far less common in the UK than it was in the early 20th century, it remains a significant cause of heart valve problems worldwide and continues to be diagnosed in British clinical practice. Rheumatic fever is an inflammatory disease that can develop after an infection with streptococcus bacteria, such as strep throat or scarlet fever. If the initial infection is not fully treated, the body’s immune system can mistakenly attack its own tissues, particularly the heart valves. This can lead to permanent damage known as rheumatic heart disease (RHD).
What We’ll Discuss in This Article
- The link between rheumatic fever and long-term heart valve damage.
- Why rheumatic heart disease remains a clinical concern in the UK.
- The primary symptoms of valve issues caused by rheumatic fever.
- How the body’s immune response leads to valve scarring.
- The differences between acute rheumatic fever and chronic valve disease.
- Essential safety guidance and when to seek medical help.
Does Rheumatic Fever Still Cause Valve Problems?
Yes, rheumatic fever remains a primary cause of acquired heart valve disease. Although its incidence has declined in high-income countries like the UK due to improved living standards and antibiotic use, it still causes ‘rheumatic heart disease’ in many individuals. The condition typically results in the thickening, scarring, and fusion of heart valve leaflets, which can lead to both stenosis (narrowing) and regurgitation (leaking) years after the initial infection.
In a clinical setting, doctors often see the effects of rheumatic fever in older adults who contracted the illness in childhood, or in individuals who have moved to the UK from regions where the disease is more prevalent. The mitral valve is the most frequently affected, followed by the aortic valve.
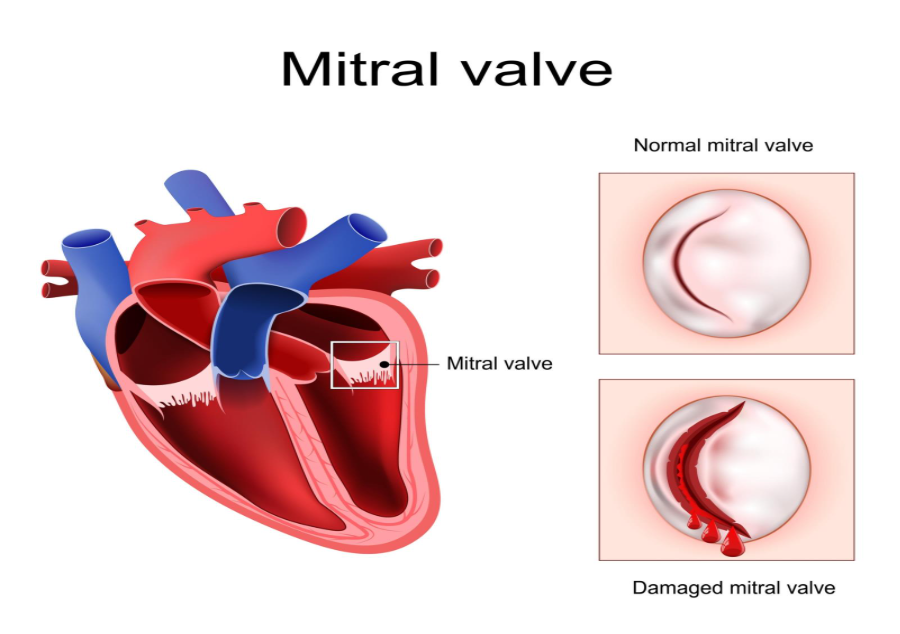
- Mitral Valve Involvement: The most common site of rheumatic damage.
- Delayed Progression: Symptoms of valve problems often do not appear until 10 to 20 years after the original fever.
- Chronic Inflammation: Even after the infection is gone, the structural changes to the valve can be permanent.
What are the Main Symptoms of Rheumatic Valve Disease?
The symptoms of valve problems caused by rheumatic fever often develop very gradually. Many people remain asymptomatic for decades until the valve damage becomes moderate or severe. Common signs include shortness of breath during activity or when lying flat, persistent fatigue, and heart palpitations. As the heart struggles to pump efficiently, fluid may build up, leading to swelling in the ankles or feet.
Because the damage is structural, it can eventually lead to complications like atrial fibrillation (an irregular heart rhythm) or heart failure.
- Dyspnoea: Shortness of breath, often the first sign of mitral stenosis.
- Chest Pain: Discomfort or tightness, particularly if the aortic valve is involved.
- Fatigue: A general sense of tiredness as the heart works harder to circulate blood.
- Heart Murmur: An unusual sound between heartbeats that a doctor can hear with a stethoscope.
What Causes Rheumatic Valve Damage?
The cause of rheumatic valve damage is an ‘autoimmune response’ triggered by a ‘Group A Streptococcus’ infection. The body produces antibodies to fight the bacteria, but because certain proteins in heart tissue look similar to the bacteria, the immune system begins attacking the heart valves. This inflammation causes the valve flaps to become inflamed, eventually leading to scarring and stiffening.
Molecular Mimicry
The immune system’s confusion is known as ‘molecular mimicry’. The antibodies designed to destroy the strep bacteria instead target the ‘endocardium’ (the lining of the heart) and the heart valves.
Leaflet Fusion
During the inflammatory phase, the edges of the valve flaps (commissures) can become inflamed and stick together. This fusion is a hallmark of rheumatic mitral stenosis, creating a ‘funnel-shaped’ opening that restricts blood flow.
Chordae Thickening
The ‘chords’ that tether the valves in place can also become thickened and shortened. This prevents the valve from closing properly, leading to regurgitation.
What are the Triggers for Rheumatic Heart Disease?
The primary trigger for rheumatic heart disease is an untreated or inadequately treated streptococcal throat infection. While not every strep infection leads to rheumatic fever, repeated infections increase the risk of an autoimmune flare-up. In individuals who already have rheumatic damage, further streptococcal infections can act as a trigger for worsening the existing valve condition.
- Untreated Strep Throat: Failing to complete a course of antibiotics for a bacterial sore throat.
- Recurrent Infections: Multiple bouts of rheumatic fever can cause cumulative damage to the valves.
- Environmental Factors: Overcrowding and limited access to healthcare can facilitate the spread of the bacteria that trigger the condition.
Differentiation: Acute Rheumatic Fever vs. Chronic RHD
It is important to differentiate between ‘acute rheumatic fever’ and ‘chronic rheumatic heart disease’ (RHD). Acute rheumatic fever is the initial inflammatory illness characterized by joint pain and fever. Chronic RHD is the permanent structural damage to the heart valves that remains long after the fever has subsided. While the acute phase is treated with anti-inflammatories, the chronic phase may eventually require surgical intervention.
| Feature | Acute Rheumatic Fever | Chronic Rheumatic Heart Disease |
| Timing | Weeks after a strep infection. | Years or decades after the infection. |
| Primary Symptoms | Fever, painful joints, skin rashes. | Breathlessness, fatigue, palpitations. |
| Target Audience | Mostly children (5–15 years). | Adults (often 30–50+ years). |
| Heart Impact | Active inflammation of heart layers. | Permanent scarring and valve narrowing. |
Conclusion
Rheumatic fever remains a significant cause of valve problems, leading to permanent structural changes known as rheumatic heart disease. While the initial infection may seem like a distant memory, the resulting scarring can cause the heart valves to leak or narrow over time. Early recognition of symptoms and a history of rheumatic fever are essential for long-term cardiac monitoring and maintaining heart health.
If you experience severe, sudden, or worsening symptoms, such as intense chest pain, sudden breathlessness, or fainting, call 999 immediately.
Is rheumatic fever contagious?
The strep infection that triggers it is contagious, but rheumatic fever itself is an autoimmune reaction and cannot be passed from person to person.
Can rheumatic heart disease be prevented?
Yes, promptly treating strep throat infections with a full course of antibiotics is the most effective way to prevent rheumatic fever and subsequent heart damage.
Why does it take so long for symptoms to appear?
The heart is very good at compensating for minor valve issues; symptoms usually only emerge once the narrowing or leaking becomes significant enough to affect circulation.
Can adults get rheumatic fever?
While it is most common in children, adults can develop rheumatic fever, especially if they have repeated untreated strep infections.
How is rheumatic heart disease diagnosed?
A doctor will usually perform an ‘echocardiogram’ (heart ultrasound) to look for the characteristic thickening and fusion of the valve leaflets.
Do I need antibiotics for life if I had rheumatic fever?
Some people require long-term ‘secondary prophylaxis’ (regular antibiotics) to prevent further infections from causing more heart damage.
Authority Snapshot (E-E-A-T Block)
This article has been reviewed by Dr. Stefan Petrov, a UK-trained physician with extensive experience in general medicine, surgery, and intensive care. Drawing on his clinical background in hospital wards and his role in medical education, this guide provides a medically accurate overview of how rheumatic fever affects heart valves. Our goal is to provide safe, factual information based on current clinical understanding to help you recognize the long-term impact of this condition.

