What is Aortic Stenosis?
The aortic valve is one of the most important components of the heart, acting as the main gateway through which oxygen-rich blood is pumped to the rest of the body. Aortic stenosis occurs when this valve becomes narrowed or obstructed, preventing it from opening fully. This restriction forces the heart muscle to work much harder to push blood through a smaller opening, which can lead to significant health complications over time. In the UK, aortic stenosis is one of the most common heart valve diseases, particularly among older adults. This article explores the causes, signs, and clinical context of this condition.
What We’ll Discuss in This Article
- The clinical definition of aortic stenosis and how it affects the heart.
- Common symptoms that may indicate a narrowing of the aortic valve.
- The primary causes, including age-related calcification and congenital factors.
- Triggers that can worsen symptoms or accelerate the condition.
- The difference between mild, moderate, and severe aortic stenosis.
- When to seek urgent medical attention for cardiac symptoms.
Understanding Aortic Stenosis and Its Effects on the Heart
Aortic stenosis is a condition where the aortic valve narrows, restricting blood flow from the heart’s main pumping chamber (left ventricle) into the aorta. This narrowing is typically caused by a buildup of calcium or scarring, which makes the valve leaflets stiff and rigid. As the opening becomes smaller, the heart must exert more pressure to circulate blood, eventually causing the heart muscle to thicken and weaken.
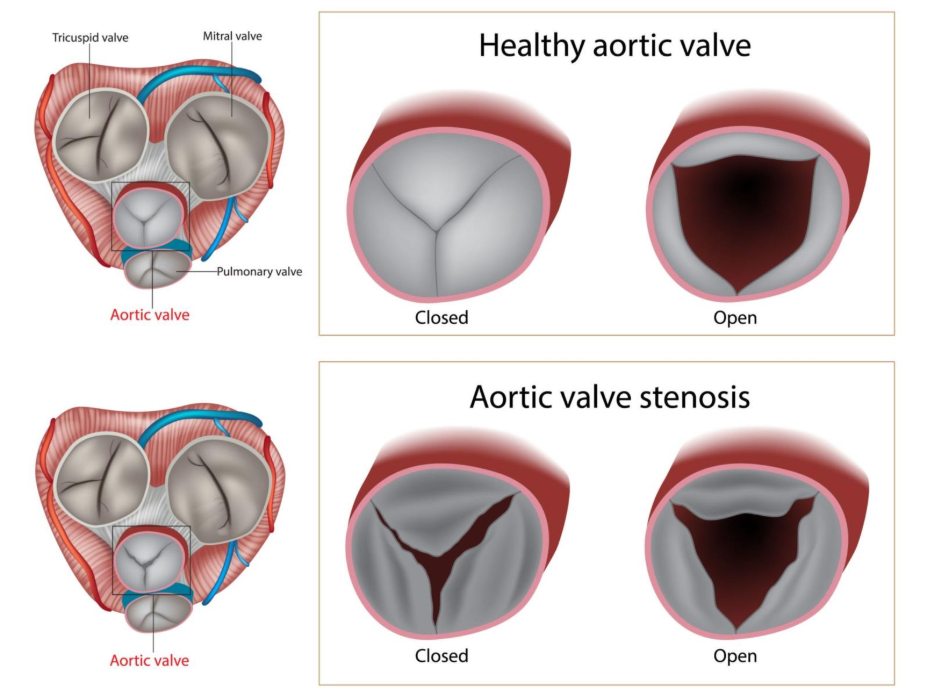
In the early stages, many people do not notice any symptoms as the heart compensates for the extra workload. However, as the stenosis progresses from mild to severe, the heart’s ability to pump enough blood to meet the body’s demands decreases, leading to symptoms like breathlessness or chest pain.
- Valve Obstruction: The physical narrowing of the ‘orifice’ or opening of the valve.
- Pressure Gradient: The difference in pressure between the heart and the aorta increases as the stenosis worsens.
- Left Ventricular Hypertrophy: The thickening of the heart muscle as it adapts to the increased workload.
- Classification: Doctors categorise the condition as mild, moderate, or severe based on ultrasound measurements.
What are the Main Symptoms of Aortic Stenosis?
The symptoms of aortic stenosis often develop gradually and may be mistaken for general signs of ageing or a lack of fitness. The three hallmark symptoms are shortness of breath (especially during activity), chest pain or tightness (angina), and feeling lightheaded or fainting (syncope). Other signs include persistent fatigue and heart palpitations, where the heart feels like it is thumping or racing.
A GP may first suspect aortic stenosis after hearing a specific type of ‘heart murmur’ through a stethoscope a harsh, whistling, or rasping sound caused by turbulent blood flow.
- Exertional Dyspnoea: Shortness of breath when performing tasks like climbing stairs or walking uphill.
- Angina: Chest discomfort that typically occurs during exercise and subsides with rest.
- Syncope: Fainting or feeling very lightheaded, which occurs because the brain is not receiving enough oxygenated blood.
- Reduced Stamina: Finding it increasingly difficult to keep up with usual daily activities.
What Causes Aortic Stenosis?
The primary causes of aortic stenosis include age-related calcium buildup (calcification), congenital heart defects, and scarring from previous infections. In older populations, the most common cause is the gradual accumulation of calcium deposits on the valve flaps over several decades. In younger individuals, the condition is often linked to a bicuspid aortic valve, where the valve is born with only two flaps instead of the usual three.
Age-Related Calcification
As we age, the constant mechanical stress on the aortic valve can cause microscopic damage. The body responds by depositing calcium a mineral found in the blood onto the valve leaflets. This process, known as ‘calcific degeneration’, eventually makes the valve flaps thick and immobile.
Bicuspid Aortic Valve
This is a congenital condition present from birth. Instead of three delicate leaflets, the valve has only two. This abnormal shape causes more turbulent blood flow, which leads to the valve wearing out and narrowing much earlier in life, often in a person’s 40s or 50s.

Rheumatic Fever
Though rare in the UK today, rheumatic fever following a childhood throat infection can cause the edges of the valve flaps to fuse together. This creates a permanent narrowing that often becomes symptomatic in adulthood.
What are the Triggers for Worsening Aortic Stenosis?
While the narrowing of the valve is a structural process, certain lifestyle and health factors can act as triggers that accelerate the condition or cause symptoms to flare up. Chronic high blood pressure (hypertension) is a major trigger, as it increases the resistance the heart must pump against. High cholesterol and smoking also contribute by increasing inflammation and speeding up the deposition of calcium on the valve.
- Hypertension: High blood pressure puts extra mechanical strain on an already narrowed valve.
- Sedentary Lifestyle: A lack of activity can make the heart muscle less efficient at managing the pressure of stenosis.
- Poor Diet: High intake of saturated fats and salt can worsen the underlying factors that lead to valve calcification.
- Infection: Developing an infection like endocarditis can cause rapid damage to a stenotic valve.
Differentiation: Aortic Stenosis vs. Aortic Regurgitation
It is important to differentiate between aortic stenosis and aortic regurgitation (a leaky valve). While both affect the same valve, stenosis involves a valve that cannot open properly, whereas regurgitation involves a valve that cannot close tightly. In stenosis, blood is blocked from moving forward; in regurgitation, blood leaks backward into the heart. Both conditions strain the heart, but they result in different changes to the heart muscle.
| Feature | Aortic Stenosis | Aortic Regurgitation |
| Primary Issue | Failure to open fully. | Failure to close tightly. |
| Blood Flow | Obstructed/Blocked. | Leaking backward. |
| Heart Strain | Pressure overload (thick muscle). | Volume overload (enlarged heart). |
| Common Cause | Age-related calcification. | Aortic root dilation or infection. |
Conclusion
Aortic stenosis is a progressive narrowing of the heart’s main valve, primarily caused by aging, congenital factors, or previous illness. While the heart can compensate for mild narrowing for a long time, the onset of symptoms like breathlessness or chest pain signals that the condition has become more serious. Regular monitoring by a cardiology team is essential to ensure that heart function is preserved and that intervention occurs at the right time.
If you experience severe, sudden, or worsening symptoms, such as intense chest pain, sudden breathlessness, or fainting, call 999 immediately.
Is aortic stenosis the same as a heart attack?
No, a heart attack is caused by a blockage in the blood vessels supplying the heart muscle, while aortic stenosis is a mechanical problem with one of the heart’s valves.
Can exercise make aortic stenosis worse?
In cases of severe stenosis, strenuous exercise can put a dangerous amount of strain on the heart; always follow your specialist’s advice regarding physical activity.
Is there a medication to clear the calcium from the valve?
Currently, there are no medications that can ‘dissolve’ the calcium once it has hardened on the valve; surgery is the only way to physically widen the opening.
How is aortic stenosis diagnosed?
The most common diagnostic tool is an ‘echocardiogram’ (an ultrasound scan of the heart), which measures the valve opening and the speed of blood flow.
Is aortic stenosis hereditary?
Some causes, such as a bicuspid aortic valve, can run in families, so it is often recommended that close relatives are screened if you have this condition.
Can you live a normal life with aortic stenosis?
Many people with mild or moderate stenosis live normal lives with regular monitoring, though lifestyle adjustments may be needed as the condition progresses.
Authority Snapshot (E-E-A-T Block)
This article was written and reviewed by Dr. Rebecca Fernandez, a UK-trained physician with extensive experience in cardiology, internal medicine, and emergency care. Drawing on her clinical background in managing acute cardiac cases and providing comprehensive inpatient care, this guide provides a medically accurate overview of aortic stenosis. Our goal is to provide clear, safe, and factual information to help you understand this common heart valve condition.


