Are oxygen therapy or breathing treatments required for pulmonary embolism?
Pulmonary embolism is a medical condition where a blood clot blocks a blood vessel in the lung, which can interfere with the body’s ability to transfer oxygen into the bloodstream. While the primary treatment involves medication to manage the clot itself, supportive therapies such as oxygen are often used to stabilize patients who are experiencing respiratory distress. This guide explains how UK healthcare professionals determine the need for breathing support and the different types of therapy used in a clinical setting.
What We’ll Discuss in This Article
- The clinical purpose of oxygen therapy in treating a lung clot.
- How doctors monitor oxygen levels to determine the need for support.
- Different methods of delivering oxygen, from nasal cannulae to masks.
- The role of advanced breathing support in severe or unstable cases.
- Why standard “breathing treatments” like inhalers are used for other conditions.
- When emergency intervention is required for breathing difficulties.
The role of oxygen therapy in pulmonary embolism
Oxygen therapy is required for patients with a pulmonary embolism when the blockage in the lung prevents the blood from picking up enough oxygen to meet the body’s needs. The NHS states that if you are admitted to hospital with a pulmonary embolism, you may be given oxygen to help with your breathing and ensure your vital organs receive an adequate supply. This treatment is supportive rather than curative, as it manages the symptoms of breathlessness while anticoagulant medications work to stop the clot from growing.
Monitoring oxygen levels and respiratory rate
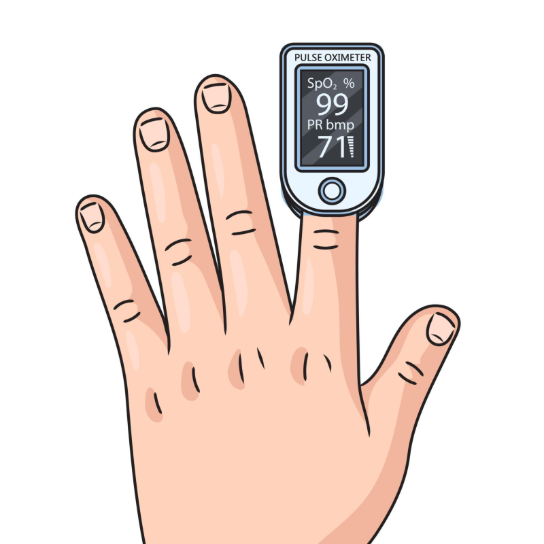
Healthcare professionals use non-invasive monitoring tools, such as pulse oximetry, to measure the saturation of oxygen in a patient’s blood and decide if therapy is necessary. A small sensor is placed on the finger to provide a continuous reading, allowing the medical team to adjust the amount of oxygen being delivered in real time. If a patient’s oxygen levels fall below a specific target range or if their breathing rate is significantly increased, oxygen therapy is initiated immediately to reduce the strain on the heart and lungs.
Methods of delivering oxygen support
There are several ways to deliver oxygen to a patient, ranging from low-flow systems to more intensive high-flow masks, depending on the severity of the hypoxia. Most patients start with a nasal cannula, which consists of two small prongs that sit just inside the nostrils, allowing them to talk and eat comfortably. If higher concentrations of oxygen are needed, a simple face mask or a non-rebreath mask with a reservoir bag may be used to ensure the patient receives a more concentrated supply of oxygen.
| Delivery Method | Description | Common Use Case |
| Nasal Cannula | Small tubes in the nostrils. | Mild breathlessness or stable patients. |
| Simple Face Mask | Mask covering nose and mouth. | Moderate oxygen requirements. |
| Non-Rebreath Mask | Mask with a reservoir bag attached. | Severe breathlessness or emergency stabilization. |
| High-Flow Oxygen | Heated and humidified high-speed air. | Significant respiratory distress or heart strain. |
Advanced breathing support for unstable cases
In rare and severe cases where a large pulmonary embolism causes the lungs or heart to fail, advanced breathing support may be required in an intensive care setting. This can include non-invasive ventilation, where a tightly fitting mask pushes air into the lungs, or mechanical ventilation, where a machine takes over the work of breathing for the patient. These interventions are reserved for high-risk situations where the blockage is so significant that the patient cannot maintain their own breathing effectively.
Differentiating pulmonary embolism from asthma or COPD
It is important to note that “breathing treatments” such as nebulisers or inhalers, which are common for asthma or chronic obstructive pulmonary disease (COPD), do not treat a pulmonary embolism. While these treatments work by opening the airways (bronchodilation), a pulmonary embolism is a problem with blood flow (perfusion) rather than a narrowing of the tubes. NICE guidelines focus on anticoagulant therapy and oxygenation for pulmonary embolism, rather than bronchodilators, unless the patient has a pre-existing lung condition that is also flaring up.
Conclusion
Oxygen therapy is a vital supportive treatment for many patients with a pulmonary embolism to ensure the body remains well-oxygenated during the recovery process. The need for this support is based on careful monitoring of blood oxygen levels and the patient’s overall respiratory effort. While most patients only require simple oxygen masks or nasal tubes, advanced support is available for more critical cases. If you experience severe, sudden, or worsening symptoms, call 999 immediately.
Will I have to go home with oxygen?
Most patients only require oxygen while they are in the hospital; once the clot begins to stabilize and their breathing improves, they are usually able to maintain safe oxygen levels on their own.
Does everyone with a lung clot need oxygen?
No, if your oxygen levels remain within the normal range and you are not in significant distress, you may not require any supplemental oxygen.
Can oxygen therapy dissolve the blood clot?
No, oxygen only helps your body cope with the symptoms; medication like anticoagulants is required to manage the actual blood clot.
Is it difficult to breathe while wearing an oxygen mask?
Most patients find that oxygen therapy actually makes it easier to breathe by reducing the feeling of breathlessness and air hunger.
Are there side effects to receiving oxygen?
Oxygen is a medical treatment and can cause dryness in the nose or throat, which is why it is sometimes humidified if used for long periods.
Authority Snapshot (E-E-A-T Block)
This guide was produced by the MyPatientAdvice Medical Content Team and reviewed by Dr. Stefan Petrov to provide clear, evidence-based information for the public. The content is strictly aligned with the clinical standards and pathways established by the NHS and NICE for the management of pulmonary embolism. Our objective is to support patient understanding of supportive hospital treatments and the importance of professional respiratory monitoring.

