Is a pulmonary embolism life threatening?
A pulmonary embolism is a serious medical condition that requires immediate assessment because it can be life threatening if the blockage in the lung is large or left untreated. It occurs when a blood vessel in the lung is obstructed by a clot that has travelled from another part of the body, usually the leg. The impact on the heart and the body’s oxygen levels makes this a critical clinical event that must be managed by healthcare professionals in a hospital setting.
What We’ll Discuss in This Article
- Why a pulmonary embolism is classified as a medical emergency.
- The physiological impact of a blockage on the heart and lungs.
- Factors that determine the severity of an individual episode.
- The importance of prompt diagnosis and starting treatment.
- Long term outlook and the risk of future blood clots.
- When to call for an ambulance and emergency clinical protocols.
Why a pulmonary embolism is a medical emergency
A pulmonary embolism can be life threatening and requires immediate medical treatment to prevent serious complications or death. It is considered an emergency because a significant blockage can suddenly stop blood from reaching large sections of the lung tissue. This not only prevents the blood from picking up oxygen but also creates a physical barrier that the heart must work against, which can lead to acute heart failure if the pressure becomes too high.
The danger of a pulmonary embolism lies in its unpredictability and the speed at which it can affect vital functions. While some smaller clots may cause milder symptoms, a large clot (known as a saddle embolus) can block the main arteries of both lungs at once. Because it is impossible for a patient to know the size or stability of a clot based on symptoms alone, UK medical guidance dictates that all suspected cases must be treated as life threatening until proven otherwise by diagnostic imaging.
The impact on heart and lung function
When a pulmonary embolism occurs, the primary issue is a mechanical obstruction that disrupts the normal flow of blood through the pulmonary circulation. The right side of the heart, which is responsible for pumping deoxygenated blood into the lungs, suddenly encounters high resistance. This can cause the right ventricle to stretch and weaken, a state known as right heart strain, which reduces the amount of blood the heart can pump out to the rest of the body.
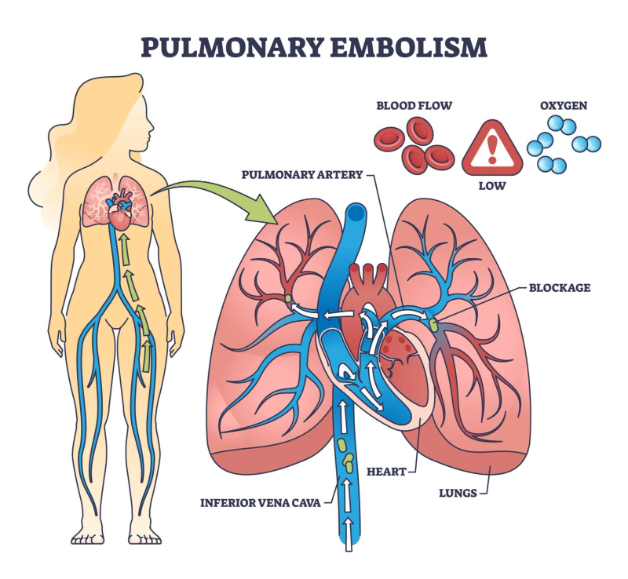
Simultaneously, the lungs cannot oxygenate the blood that is blocked behind the clot. This leads to a drop in blood oxygen levels, forcing the person to breathe much faster and the heart to beat more rapidly to compensate. If the blockage is extensive, the lack of oxygen can affect other organs, including the brain and kidneys. In some instances, the area of the lung deprived of blood may suffer tissue death, which further complicates the patient’s recovery and respiratory capacity.
Factors determining the severity of the condition
The severity of a pulmonary embolism and the risk to life are largely determined by the size of the clot and the patient’s underlying health. A massive embolism that blocks a major artery is immediately life threatening because it can cause a sudden collapse in blood pressure. Conversely, smaller clots that affect only the peripheral branches of the pulmonary system may be less immediately dangerous but still require urgent treatment to prevent further clots from forming.
Individual health factors also play a significant role in how the body handles a blockage. A person with pre-existing heart or lung disease has less “reserve” and may become critically ill more quickly than a younger, otherwise healthy individual. Age, the presence of cancer, and previous history of blood clots are all factors that doctors use to assess the clinical risk. The goal of emergency care is to stabilize the patient’s oxygen levels and blood pressure while preventing the existing clot from growing larger.
The importance of prompt treatment
Treatment for a pulmonary embolism usually involves anticoagulant medicines, which help stop the blood clot from getting bigger while your body slowly dissolves it. Starting these medications promptly is the most effective way to reduce the risk of the condition becoming fatal. Anticoagulants, or blood thinners, do not break down the clot themselves but they prevent new clots from forming and stop the current one from migrating further into the lung.
In the most severe, life-threatening cases where the patient is unstable, more intensive treatments may be required. This can include thrombolytic “clot-busting” drugs that work to dissolve the blockage rapidly or surgical procedures to physically remove the clot. Because these intensive treatments carry their own risks, such as internal bleeding, they are typically reserved for patients whose lives are at immediate risk. Early intervention in a hospital environment significantly improves the chances of a full recovery.
Conclusion
A pulmonary embolism is a life-threatening condition that requires urgent medical attention to prevent heart strain and restore oxygen levels. The risk to life depends on the size of the blockage and how quickly treatment with anticoagulant medication is started. Understanding that sudden breathlessness or chest pain can signal a major emergency is vital for patient safety and successful clinical outcomes.
If you experience severe, sudden, or worsening symptoms, call 999 immediately.
Can you survive a pulmonary embolism without treatment?
While some very small clots might be managed by the body’s natural systems, a pulmonary embolism is too dangerous to leave to chance. Without medical treatment, there is a high risk that more clots will form or the existing one will move, potentially leading to a fatal event.
How long does the danger last after a diagnosis?
The highest risk period is usually the first few days after the embolism forms. Once you are stabilized on anticoagulant medication, the risk of the clot growing or a new one forming decreases significantly, although you will need to remain on treatment for several months.
What is a “silent” pulmonary embolism?
A silent pulmonary embolism refers to a blockage that does not cause obvious symptoms like breathlessness or pain. However, even if it is silent, it can still cause underlying strain on the heart and indicates a serious problem with blood clotting that needs medical management.
Is the damage to the lungs permanent?
In many cases, the lungs can recover fully once the clot is dissolved and blood flow is restored. However, if a significant area of lung tissue died during the blockage (infarction), there may be some localized scarring, though this does not always affect long-term breathing.
Why is deep vein thrombosis related to this risk?
Deep vein thrombosis is the most common source of the clots that cause pulmonary embolism. If a clot in the leg is not treated, it remains a “ticking clock” that could break free at any time and travel to the lungs, making leg symptoms an important warning sign.
Can children get a life-threatening pulmonary embolism?
While much rarer than in adults, children can develop pulmonary embolisms, usually due to underlying medical conditions, surgery, or long-term intravenous lines. The symptoms and the need for emergency treatment are the same regardless of the patient’s age.
Authority Snapshot
This article was developed to inform the public about the life-threatening nature of pulmonary embolism and the necessity of emergency care. It has been authored by Dr. Stefan Petrov, a UK-trained physician, and reviewed by the MyPatientAdvice clinical team. All information provided is strictly aligned with NHS and NICE clinical safety guidelines to ensure accuracy and public safety.

