Can stress-management reduce risk of chronic fatigue or pain?
In the United Kingdom, medical research increasingly highlights the role of chronic stress as a primary ❛perpetuating factor❜ in the development of myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) and fibromyalgia. While stress itself is rarely the sole cause, it acts as a significant biological load that can prevent the body from recovering after a viral infection or physical trauma. The NHS and 2021 NICE guidelines acknowledge that managing stress is not just about emotional wellbeing; it is a vital strategy for regulating the autonomic nervous system and preventing the state of ‘high alert’ that leads to chronic pain and exhaustion.
What We’ll Discuss in This Article
- The ‘Allostatic Load’: How cumulative stress impacts the body
- The ‘Fight or Flight’ response and the Vagus nerve
- Why stress ‘turns up the volume’ on pain signals
- Stress as a trigger for post-viral syndromes
- UK-based techniques: Mindfulness, pacing, and sleep hygiene
- The role of ‘Cognitive Energy’ management
Understanding the ‘Allostatic Load’
In UK clinical practice, the term Allostatic Load refers to the ‘wear and tear’ on the body that accumulates when an individual is exposed to repeated or chronic stress. When your body is constantly dealing with stressors, whether they are emotional, physical, or environmental, it remains in a state of physiological emergency.
If a major trigger occurs (such as a severe virus or an injury) while your allostatic load is already high, your system may lack the resilience to reset. This can result in the ‘on’ switch for the stress response getting stuck, leading to the cellular and neurological dysfunction seen in ME/CFS and fibromyalgia. Reducing stress lowers this ‘background noise,’ providing your body with a better chance to heal from acute events.
The nervous system and the Vagus nerve
Stress management is essentially the practice of training your nervous system to move out of the Sympathetic (fight or flight) state and into the Parasympathetic (rest and digest) state. The primary actor in this process is the Vagus nerve.
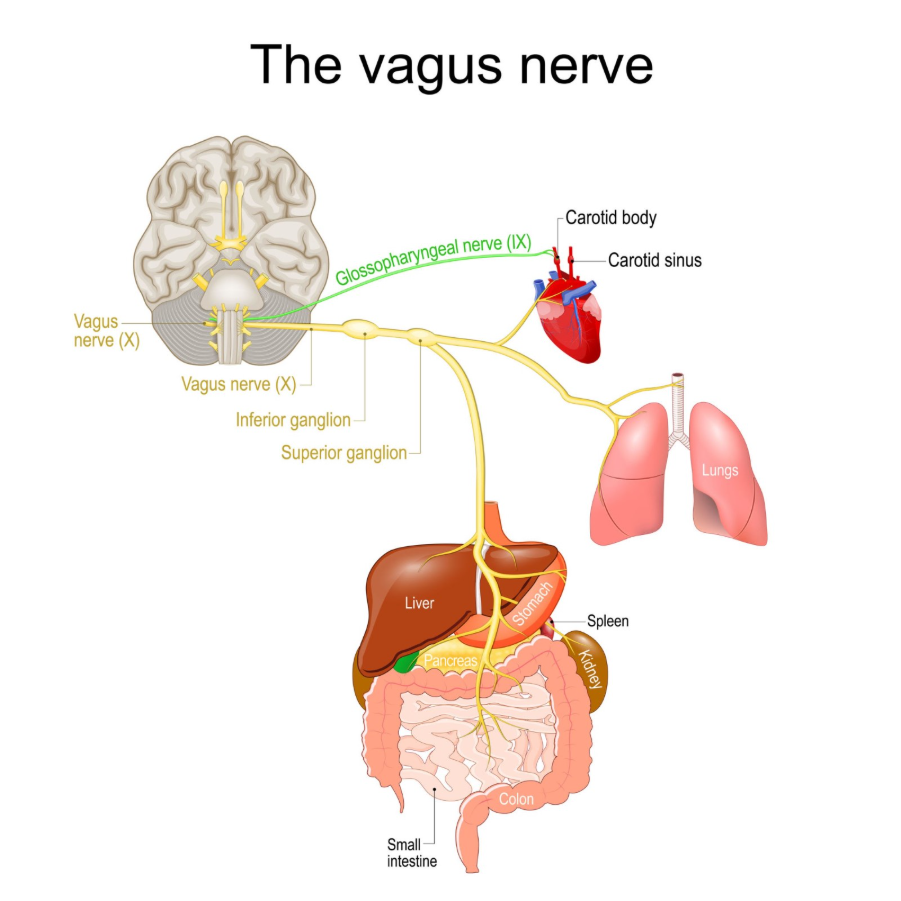
If the Vagus nerve is ‘toned’ through stress-management techniques, it can more effectively signal the heart, lungs, and digestive system to calm down. In people with chronic fatigue or pain, the Vagus nerve often underfunctions, leaving the body in a state of permanent tension. By proactively managing stress, you help maintain ‘Vagal tone,’ which keeps your immune system and energy production more stable.
Why stress ‘turns up the volume’ on pain
For those at risk of fibromyalgia, stress management is a direct preventative tool against central sensitisation. When the brain is under stress, it becomes hyper-vigilant. It begins to scan the body more intensely for threats, which means it starts to interpret normal signals, like the pressure of clothing or a cool breeze, as pain.
By practising stress reduction, you are effectively ‘lowering the volume’ on the brain’s pain-processing centres. In the UK, the NICE guidelines for chronic pain emphasise that reducing emotional distress is a key component in preventing a temporary pain event from becoming a permanent, widespread condition.
Stress as a catalyst for post-viral syndrome
A significant number of ME/CFS cases in the UK begin after a viral infection, such as Glandular Fever or COVID-19. Research suggests that if a person is under intense stress at the time of the infection, their immune system may over-react or fail to return to baseline.
Effective stress management ensures that your HPA axis (the system that coordinates your stress response) is balanced. A balanced HPA axis allows the immune system to fight a virus and then ‘stand down,’ rather than remaining in a state of chronic inflammation that fuels long-term fatigue.
Conclusion
Managing stress is a powerful and evidence-based way to reduce the risk of chronic fatigue and pain. It is not about ‘thinking yourself healthy,’ but about managing the biological environment of your body. By lowering your allostatic load and supporting your Vagus nerve, you provide your nervous system with the stability it needs to resist the ‘sensitisation’ that leads to fibromyalgia and ME/CFS. In the UK, stress management is viewed as a foundational skill for long-term health protection. In 2026, the goal is to intervene early, using pacing, mindfulness, and lifestyle adjustments to ensure that the stresses of modern life do not become the triggers for a lifetime of chronic illness.
If you experience severe, sudden, or worsening symptoms, call 999 immediately.
Does stress management mean the illness is ‘all in my head’?
No. ME/CFS and fibromyalgia are physical, biological conditions. Stress management is used because stress has physical and biological effects on your heart, hormones, and nerves.
Can stress management cure existing CFS?
While it may not be a ‘cure,’ it is a vital part of management. Reducing the ‘stress load’ often expands a person’s ‘energy envelope,’ allowing for a better quality of life.
What is ‘Vagal Tone’?
This refers to the activity of your Vagus nerve. High Vagal tone is associated with better heart rate variability and a more resilient stress response.
Should I use CBT for stress?
Under UK NICE guidelines, CBT is recommended as a supportive tool to help manage the distress of being ill, rather than as a treatment for the fatigue itself.
How does ‘Pacing’ help with stress?
Pacing reduces ‘physical stress’ on the body. By not over-exerting yourself, you prevent the adrenaline surges that keep your nervous system in ‘fight or flight’ mode.
Is ‘Brain Fog’ affected by stress?
Yes. High levels of cortisol (the stress hormone) can impair the function of the hippocampus, the part of the brain involved in memory and word-finding.
Can mindfulness really change my nerves?
Yes. Studies show that regular mindfulness can actually change the grey matter in areas of the brain associated with stress and emotional regulation, leading to a calmer baseline.
Authority Snapshot (E-E-A-T Block)
This article provides a medically accurate overview of the role of stress management in preventing chronic fatigue and pain within the UK. It was prepared by the MyPatientAdvice team and reviewed by Dr. Stefan Petrov to ensure alignment with current NHS standards and the 2021 NICE guidelines. The goal is to encourage proactive health management through evidence-based relaxation and pacing.

